Damage to the kidneys can result in chronic kidney disease. As this condition progresses it moves across five different stages. This article focuses on stage 3 kidney disease. Read on to learn about what it is, how you know you have it, how to treat it, and what you need to know to stop the progression of kidney decline.
Table of Contents
What is Chronic Kidney Disease?
Chronic kidney disease or CKD for short is a condition that affects 37 million American adults according to the National Kidney Foundation.
It is a disease that affects the health of the kidneys. Over time the kidneys get worn out and are longer be able to function properly.
What is Stage 3 Kidney Disease?
There are five stages of kidney disease. It starts with mild kidney damage in stage one. If this condition goes unmanaged it will progress up to stage 5. Also known as end stage renal disease (ESRD).
This is when kidney failure sets in. The kidneys no longer work and dialysis is required to filter the blood.
This article will mainly focus on third stage kidney disease. This is where disease progression hits the middle of the spectrum.
If you’re wondering, is stage 3 kidney disease serious? Yes, it is. Stage 3 is worse than stage 1 but doesn’t have as much damage as stage 4 and 5.
Damage has been done to the kidneys that cannot be repaired but they still can function.
In stage 3 there is still time to preserve kidney health. It may also prevent someone from losing all kidney function and needing dialysis.

What Causes Stage 3 Kidney Disease To Occur?
Stage 3 kidney disease is not something that just comes on suddenly. Instead, it progresses over time due to chronic kidney disease.
Health Conditions that Impact Stage 3 Kidney Disease
This disease occurs when there is damage to the kidneys. Conditions that may lead to CKD are
- Diabetes
- High blood pressure
- Glomerulonephritis
- Inherited diseases
- Autoimmune disorders

Diabetes
When blood sugar becomes too high diabetes sets in. High blood sugar can damage blood vessels in the kidneys leading to poor kidney function.
High Blood Pressure
The kidneys are needed for blood pressure regulation. Uncontrolled high blood pressure weakens and damages the kidney. Because of this, they will not be able to excrete wastes.
This causes fluid imbalances which lead to hypertension. High blood pressure causes damage to kidney blood vessels resulting in further water retention.
Glomerulonephritis
Glomerulonephritis is a group of disorders that inflame and damage the kidney’s filtering units. This is the third leading cause of kidney disease.
Inherited Diseases
Some people are born with a condition that causes damage to the kidneys. These include
- Polycystic kidney disease
- Alport syndrome
- Tuberous sclerosis
- Von Hippel Lindau disease
- Thin Basement Membrane Disease
- Gitelman and Bartter Syndromes
- Lowe Syndrome
- Hereditary Interstitial Kidney Disease
- Fabry Disease
- Nephronophthisis
- Nephrogenic diabetes insipidus
Autoimmune Conditions
Autoimmune conditions occur due to a hypersensitive immune system.
In these conditions, the body sees its cells as foreign invaders and will attack. Cell damage and inflammation will then occur.
Autoimmune conditions that cause problems for the kidneys include Lupus and Good Pasture Syndrome.
An autoimmune kidney disease is known as IgA nephropathy.
How is Stage 3 Kidney Disease Diagnosed?
You may be wondering what happens in stage 3 kidney disease? Get the details here.
This is the first stage that the disease can be detected by a clinical diagnosis. A blood and urine test will tell how well the kidneys are functioning.
What Measures Kidney Function?
Creatinine levels measure kidney function. Creatinine is a waste product that is produced from the normal wear and tear on muscles in the body. Therefore, the level of creatinine tells how well the kidneys are functioning.
The kidneys are responsible for getting rid of creatinine. This creatinine clearance shows how much creatinine has passed through your kidneys into your urine.
Estimated Glomerular Filtration Rate (EGFR) Tells Your Kidney Disease Stage
Another name for creatinine clearance is the estimated glomerular filtration (eSGF) or estimated glomerular filtration rate (eGFR).
This number is the most accurate way to measure kidney function. It is based on the results of the creatinine clearance, your age, body size, and gender.
Your doctor can calculate the eGFR to determine the stage of kidney disease. The lower the number the worse the kidneys are functioning.
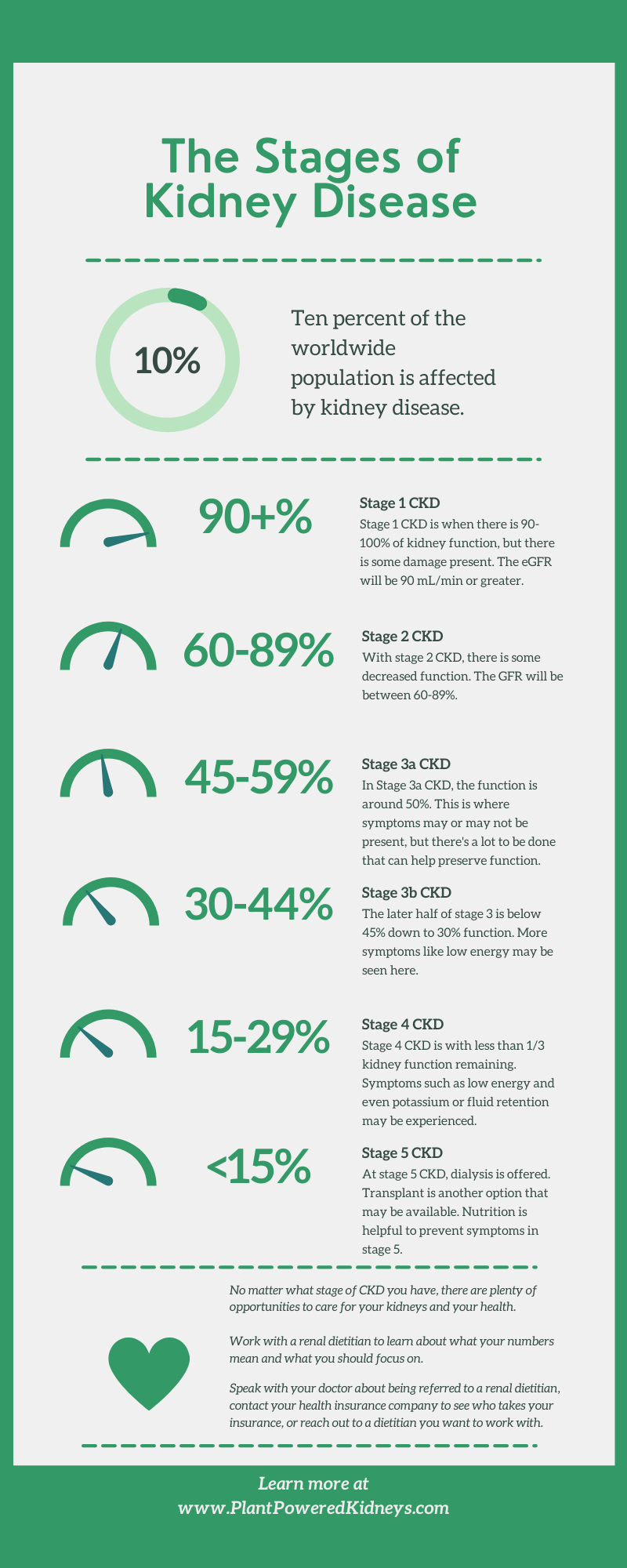
See below for the breakout of eGFR based on each stage of kidney disease.
CKD Stage 1 eGFR
CKD stage 1 is when there is still 90 to 100 percent of kidney function left. This stage has kidney damage with normal kidney function. The eGFR is at 90 mL/min or higher.
CKD Stage 2 eGFR
CKD stage 2 is when the kidneys have 60 to 89 percent of function. This stage has kidney damage with mild loss of kidney function. The eGFR falls between 60 and 89 mL/min.
CKD Stage 3 eGFR
Stage 3 kidney has two stages: 3A and 3B.
CKD Stage 3A
The 3A stage of kidney disease is when there is mild to moderate loss of kidney function. At this point, the kidneys are functioning between 45 to 59 percent. The eGFR for stage 3A is between 45 and 59 mL/min.
CKD Stage 3B
The 3B stage of kidney disease is when there is moderate to a severe loss of kidney function. The kidneys are operating at only 30 to 40% capacity. The eGFR in stage 3B is between 30 and 40 mL/min.
CKD Stage 4 eGFR
In CKD stage 4, there is severe loss of kidney function. The kidneys perform between only 15 and 29% capacity. The eGFR runs between 15 and 29 mL/min.
CKD Stage 5 eGFR
CKD stage 5 is when kidney failure or end-stage renal disease (ESRD). This means that there is less than 15% of kidney functioning happening. The eGFR is less than 15 mL/min. This stage can require dialysis or a kidney transplant.
Risk factors
Like chronic kidney disease having another underlying health condition may increase your chances of moving into stage 3.
Risk factors for CKD3 include the following:
- Age
- History of diabetes
- History of hypertension
- Smoking
- Autoimmune disorders
- Family history of kidney failure
- High cholesterol
- Atherosclerosis
- Kidney stones
- Urinary Tract Infections (UTIs)
- Enlarged prostate
- Obesity
- A genetic disorder that produces cysts in and/or damages the kidneys
- A kidney infection
- Scleroderma
- Liver disease
- A drug that is toxic to the kidneys
- Conditions that inflame the kidney
- Heavy metal poisoning (lead poisoning)
- Conditions that damage blood vessels in the kidneys (hemolytic uremic syndrome)
- Conditions that damage arteries in the kidneys (renal artery stenosis)
CKD is also more prevalent among certain races and ethnicities. These include:
The risk of diabetes and heart disease is high among these groups of people. When these conditions go unmanaged they can manifest into stage 3 of chronic kidney disease.

Symptoms
The early stages of CKD often do not show any symptoms. So the health of the kidneys will be slowly declining but you will have no idea that it is happening.
Luckily, some symptoms occur during the middle stage of CKD.
Stage 3 kidney disease symptoms include:
- Protein in the urine
- Insomnia
- Fatigue
- Brain Fog
- Dry skin
- Itchy skin
- Frequent urination
- Blood in the urine
- Foam in the urine
- Puffiness around the eyes
- Swelling in ankles and feet
- Muscle weakness, cramps, or pain
- Loss of appetite
Complications
Complications can arise from unmanaged kidney disease. However, they are not specific to any particular stage. Alternatively, they can occur throughout the disease during any or all of the stages of CKD.
As kidney function declines, wastes cannot be not properly excreted. As a result, they will build up in the body.
When these levels become too high people often feel sick and the following complications may develop:
- Anemia
- High blood pressure
- Cardiovascular disease
- Diabetes
- Mineral and bone disorders
- Changes in Nutritional Needs
- Nerve damage and neurological conditions
- High cholesterol and atherosclerosis
- Electrolyte Disorders (Salt and water retention)
- Metabolic acidosis
Anemia
There are many causes of anemia but when it comes to kidney disease the most likely reason is due to a lack of the hormone erythropoietin. This compound is created by the kidneys and produces red blood cells.
So when the kidneys are not working properly erythropoietin is in low supply. This means fewer blood cells are being made and anemia may develop.
Anemia that goes untreated can result in cardiovascular disease. Anemia can also cause cognitive decline and increase the risk of stroke for those with CKD.
During this condition, less oxygen is delivered to the brain. This can cause serious damage.
One of the ways to prevent anemia is to focus on an iron-rich diet. Read this article for iron-rich foods.
High Blood Pressure
High blood pressure is a complication of stage 3 kidney disease. Hypertension can damage blood vessels in the kidneys. Impaired blood vessels will impact kidney function.
As a result, the kidneys will not be able to remove extra fluid and waste from the body.
More fluid means a shift in blood pressure balance. This will increase blood pressure and put more pressure on the kidneys. Therefore, uncontrolled blood pressure can lead to kidney failure.
Patients with hypertension will have a greater risk of getting cardiovascular disease. A high mortality rate is also associated with having too high or too low blood pressure.
Cardiovascular Disease
Cardiovascular risk occurs with even mild to moderate kidney dysfunction. This means that at stage 3 you could potentially develop heart disease.
One heart complication in stage 3 CKD is left ventricular hypertrophy (LVH). The risk for this disease increases when kidney function and eGFR decline. Other conditions that play a role in this condition are anemia and hypertension.
Diabetes
Some people with kidney disease may develop diabetes. Damaged kidneys will have trouble removing the waste product urea from the blood.
In animal cells, a build-up of this compound caused inflammation and also inhibited the activity of phosphofructokinase 1 (PFK-1).
PFK-1 is an enzyme that helps produce insulin.
Less insulin means there will be more sugar in the blood. Unmanaged high blood sugar levels can result in diabetes.
Mineral and Bone Disorders
CKD can lead to abnormalities in how the kidneys metabolize nutrients. The kidney is unable to make enough vitamin D.
Low levels of vitamin D can lead to poor bone health. These disorders increase cardiovascular disease risk and death.
Phosphorus levels become elevated during stage 3 of kidney disease. Weakened kidneys also have trouble removing phosphorus from the body.
Calcium levels will then fall. This tells the brain to secrete the parathyroid hormone (PTH) to stop the body from excreting calcium.
Secondary hyperparathyroidism (sHPT) then occurs. It is when the body takes calcium from the bones. It can start happening even before phosphorus levels become abnormal.
These changes in calcium, phosphorus, PTH, vitamin D affect bone formation. When the eGFR drops below 60 mL/min (stage 3) changes in bone structure will occur this is known as renal osteodystrophy.
It occurs due to bone turnover and consists of four types:
- Osteitis fibrosa cystica (high bone turnover with secondary hyperparathyroidism)
- Osteomalacia (low bone turnover and low vitamin D)
- Adynamic bone disorder (low bone turnover due to suppression of the parathyroid)
- Mixed osteodystrophy (both high and low bone turnover)
Bone turnover is when the body takes calcium from the bone and moves it to the blood or kidneys.
It can be high or low depending on how many osteoclasts or bone-breaking cells are present.
High bone turnover is when many osteoclasts are present. Low bone turnover is when there are a normal or reduced number of osteoclasts.
Nutritional Issues
Kidney disease can affect digestion of nutrients including:
- Protein
- Water
- Salt
- Phosphorus
These changes will alter nutritional requirements. If not handled properly someone may experience malnutrition.
Changes in nutrient needs will also cause dietary restrictions. These metabolic changes can lead to poor intestinal absorption.
Many people with CKD often eat less of the vitamins folate, iron, and pantothenic acid.
Also, some people will experience an extreme case of altered metabolism with a build-up of uremia in the blood.
Known as uremic malnutrition, this condition is when the body does produce enough energy, even if a person is eating enough protein and carbs.
An early warning sign of uremic malnutrition is when the daily protein intake is less than 0.75 grams per kilogram of body weight (in those not on a low protein diet).
Maintaining nitrogen balance is important for those with kidney dysfunction to prevent these nutritional issues.
Nutrient deficiencies from these changes in metabolism can cause problems like anemia, cardiovascular disease, and metabolic imbalances.
Nerve Damage and Neurological Conditions
Nerves carry messages between your brain and other parts of the body. When CKD and coexisting conditions like diabetes go unmanaged nerve damage and other neurological conditions.
Up to 70% of CKD patients are at risk for nerve dysfunction.
Damaged nerves will stop sending signals and you may end up with a tingling or numbness in the hands and feet. This condition is called peripheral neuropathy.
Typical causes of peripheral neuropathy include high blood sugar, high PTH, and the accumulation of glycotoxins or advanced glycation end products AGE’s.
AGE’s are in processed foods. They also can arise naturally from digestion. These compounds are inflammatory. An accumulation of AGEs’ will cause oxidative stress and nerve damage. People can have AGE’s whether or not they have diabetes.
Elevated PTH levels, high uremic toxins, and electrolyte imbalances also play a role in the development of nerve damage.
Aside from the loss of feeling, there are neurological conditions that affect digestion and cognition.
Autonomic neuropathy is a disorder that affects the autonomic nervous system. This is the body system that works in the background without a conscious effect. Damage to this system slows how food travels through the digestive tract causing indigestion and other digestive problems.
Neurological problems are common in CKD. They affect all parts of the central nervous system and cause poor cognition or confusion.
Causes of neurological conditions are often related to
- Stroke
- Damage to the brain/nerves
- Hypertension
- Electrolyte disturbances
- Being over medicated
- Uremia toxins
- Anemia
- Elevated PTH levels
High Cholesterol
High cholesterol is a complication of unmanaged kidney disease. If left untreated it can further weaken kidneys. People with high total cholesterol or reduced HDL “good” cholesterol were more likely to have a lower eGFR indicating weaker kidney function.
This shows the potential link between cholesterol and kidney function. Improving your cholesterol levels may prevent the progression of CKD.
Lifestyle, medical, and nutrition interventions control cholesterol levels. Getting adequate exercise, quitting smoking, and managing stress are other things that can help lower cholesterol.
Medications are also prescribed for lowering cholesterol. However, it is best to start with diet and lifestyle changes. Learn more about what dietary changes can help improve cholesterol levels below.
Atherosclerosis
White blood cells will mobilize to heal blood vessels damaged by poor kidney function. As a result, plaque will form on the arterial wall. Just like with regular blood vessels atherosclerosis can occur in the kidneys.
Atherosclerosis affected 50% of patients with stage 3 kidney disease. People with an eGFR value below 60 mL/min are at risk for cardiovascular disease.
Risk factors for atherosclerosis include
- Hypertension
- High cholesterol
- Diabetes
- Age
- Being a smoker
- Metabolic acidosis
- Calcium and phosphate dysfunction
- Excessive blood clotting
- Inflammation
- Oxidative Stress
Electrolyte Disorders (Salt and Water Retention)
In CKD often there are imbalances in fluid and electrolytes. These minerals are in the blood. They regulate acid balance along with nerve and muscle function
They consist of
Hyperkalemia is the most common electrolyte disorder in CKD. This is when there is too much potassium in the blood.
As kidney function wanes, they become unable to regulate water. As a consequence, disturbances in sodium will also occur. A risk for a sodium imbalance is prevalent in stage 3 of CKD.
Having both too little and too much sodium has been seen in stage 3 CKD. The most common occurrence is excess sodium. Why this happens is not exactly certain.
Fluid retention causes the following to happen
- Swelling in the hands, arms, feet, and ankles
- Hypertension
- Cardiovascular disease especially LVH
Altered levels of sodium, calcium, and magnesium can harm the nervous system and may cause brain dysfunction.
Mineral disturbances tend to worsen as CKD progresses so managing it now is important to prolong your health. Electrolyte disorders can also contribute to uremia.
Uremia
The word “uremia” means urine in the blood. Uremia occurs when there is declining renal function. Normally common in renal failure, uremia may also manifest in stage 3 kidney disease.
As the kidneys decline they become unable to properly filter wastes. Urine metabolites and other toxins buildup in the blood. Symptoms of uremia include
- Loss of appetite and anorexia
- Fatigue
- Extreme weight and muscle loss
- Itching
- Nausea
- Restless leg syndrome
- Sleep disturbances
- Sexual dysfunction
- Brain fog
Uremia can also damage the central nervous system. Uremic neuropathy can occur as a result. It causes a loss of sensation in the limbs.
Uremia is also responsible for brain damage and may affect cognition. Toxic compounds like cystatin-C can cause amyloid plaque to form in the brain. Reduced brain function can result from high levels of this compound.
There are also indirect effects of uremia. These include:
- Inflammation
- Blood vessel damage
- Atherosclerosis
Metabolic Acidosis
As kidney function declines, they lose the ability to neutralize the acid in the body. Too much acid puts the body at risk for metabolic acidosis. High levels of acid are harmful. If unmanaged this condition can lead to
- Muscle breakdown
- Poor endocrine hormone function
- Low pituitary function
- Bone disease
Learn more about metabolic acidosis in this article about potential renal acid load here.
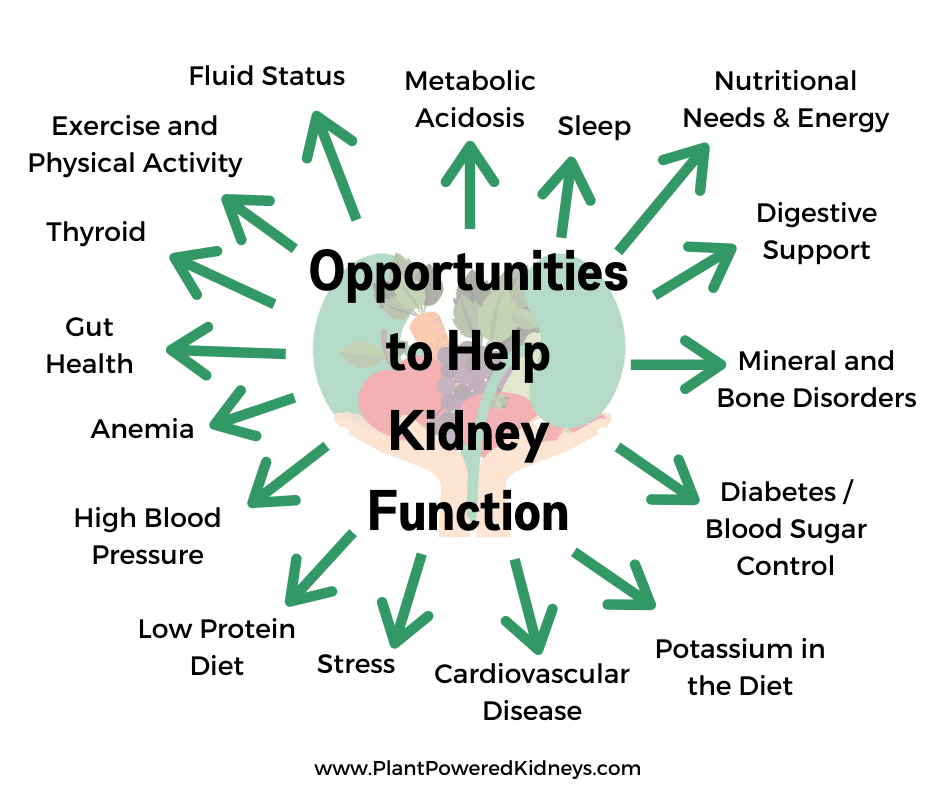
What can you do for Stage 3 Kidney Disease?
While CKD is not curable there is still a lot you can do to preserve your kidney function. Kidney care should be taken as soon as CKD has been discovered.
Kidney patients should put into place a health care team. Help from professionals will enact medical and nutritional interventions that will help to preserve kidney health and prevent disease progression.
When Should You See a Nephrologist?
When you are having renal problems you should see a kidney doctor known as a nephrologist. They are trained to manage conditions affecting the kidneys.
People without kidney disease should also seek the help of a nephrologist when they are having symptoms of kidney dysfunction including:
- Fatigue
- Sleep problems
- Changes in urination
- Family history of kidney problems and kidney disease
- High blood pressure
- Diabetes
- Heart disease
- An inherited condition that leads to kidney disease
- A lot of blood in the urine
- A lot of protein in the urine
- Recurring kidney stones
If you are not already seeing someone about your kidney disease, your primary care doctor can refer you to a local nephrologist. Or you can find one through your insurance company.
When Should You See a Renal Dietitian?
Nutrition plays a large role in kidney function. So be sure to enlist the help of a dietitian as part of your kidney management team.
These health professionals are responsible for diagnosing the root cause of the nutritional problems as well as assessing your overall health status.
Renal dietitians (RDs) are nutrition professionals specialized in kidney health. They are experts when it comes to renal nutrition. They cater specifically to individuals with kidney dysfunction and CKD.
Renal RDs provide medical nutrition therapy (MNT) to clients suffering from CKD and other kidney issues. They examine
- Lab results
- Medication lists
- Protein and calorie intake
- Albumin levels
- Potassium levels
They also make sure clients are getting adequate nutrients and adhering to any potential nutrient restrictions.
Nutrition is one of the few things that a person with kidney disease can control. MNT can treat any potential nutrition deficiencies as well as help to stop your CKD from progressing into stage 4.
It is so important for patients to incorporate help from a professional who can create an individualized nutrition action plan to help them preserve kidney function, feel better, and live longer.
Those with CKD need diet therapy. Be sure to make an appointment with a renal RD as soon as a kidney problem is diagnosed. You can use this article to learn about using your health insurance to find a dietitian.
Renal Dietitians Also Help with Other Kidney Dysfunction
People should also see a renal dietitian is when they are experiencing other signs of kidney dysfunction such as:
- Decline in kidney function
- Presence of kidney stones
- Protein in the urine
- High potassium levels
- High phosphorus levels
- You have diabetes as a result of kidney disease
- The presence of high blood pressure
- When you have questions about kidney nutrition
Your nephrologist or medical doctor should be able to help you find a renal dietitian that will take your insurance. Otherwise, you can search for a local dietitian in the National Kidney Foundation directory.
Before Seeing A Dietitian
Before seeing a dietitian be sure to have the following:
- Preliminary evaluation (ultrasound, screening serologies)
- Patient history with renal function measurements and urine albumin
- The reason you are seeing the RD
Treatments Available for Stage 3 Kidney Disease
There are nutritional, lifestyle, and medical treatments available for stage 3 kidney disease. Medical treatments will come from your doctor. Your renal dietitian will give you nutrition treatments. Both your doctor and dietitian may give you lifestyle recommendations.
Medical Treatments for Stage 3 Kidney Disease
Often your doctor may prescribe medicines to lower blood pressure, cholesterol, and control diabetes, and other coexisting conditions.
For patients in stage 3 CKD with an eGFR below 60 mL/min, certain drugs may no longer be given because they have the potential to damage the kidneys. These substances may not be able to be eliminated and will build up to toxic levels in the body. They include:
- Pethidine
- Methotrexate
- Enoxaparin
- Metformin
- Glibenclamide
- Gimepiride
- Lithium
The dose of medicine should also be adjusted for kidney function when someone’s eGFR is below 60 mL/min. This will prevent further damage to kidneys from high potassium. These include:
- ACE inhibitors
- AT1 blockers
- Renin inhibitor aliskiren
- Spironolactone
If you’re wondering how your medications can affect your kidney function it is best to talk with your doctor to know what is right for you.
Lifestyle Treatments for Stage 3 Kidney Disease
LIfestyle treatments can be prescribed by both your medical doctor and renal dietitian. They include:
- Quit smoking
- Get daily exercise
- Get enough sleep
- Maintain a healthy weight
- Control blood pressure
- Control blood sugar
- Avoid excessive pain medicine that harms the kidneys
- Avoid too much alcohol
Some of these tips fall into nutritional treatment as well.
Nutritional Treatments for Stage 3 Kidney Disease
Nutritional treatments include looking at the diet and seeing where things may need to be adjusted. This will tell you what foods are helpful and harmful to the kidneys. These treatments can help to
- Reduce blood pressure
- Lower cholesterol
- Lower blood sugar
- Maintain a healthy weight
Nutritional Treatments to Manage Stage 3 Kidney Disease & Prevent Further Damage
In this section, we will go into greater detail about how to optimize nutrition status to manage stage 3 and prevent further kidney damage. We will discuss
- Managing existing conditions and complications
- Labs to monitor
- Nutrients to monitor
- Foods to avoid
- What foods to eat
Curious what a stage 3 kidney disease diet plan looks like? Get a free 6-day meal plan with recipes and grocery list below!
Manage Pre-Existing Conditions and Complications
Good nutrition can be helpful to improve complications and conditions in kidney disease. We will discuss how changes in the diet may help improve cardiovascular disease, high blood pressure, cholesterol, diabetes, anemia, nerve damage, uremia, electrolyte imbalances, metabolic acidosis, and weight management.
Nutrition for Cardiovascular Disease
The risk of cardiovascular disease can be reduced by controlling the following:
- Blood pressure
- Diabetes
- Cholesterol
- Potassium levels
- Calcium levels
- Phosphorus levels
- Anemia
- Bone disorders
- Nerve damage
- Uremia
Nutrition for Hypertension (High Blood Pressure)
Having blood pressure under 130/85 mm Hg is recommended for all stages of kidney disease. Those whose protein excretions are greater than 1 gram per 24 hours should aim for a blood pressure that is under 125/75 mmHg.
Maintaining a healthy lifestyle can lower blood pressure. This is done through
- Having a nutritious diet
- Having a healthy weight
- Lowering salt intake
- Getting daily exercise
- Taking blood pressure medication if needed
One easy thing you can do to lower blood pressure is cut back on your salt intake. Kidneys are responsible for controlling the sodium levels in your body. When you have poor kidney function cutting back on sodium can prevent fluid buildup, swelling, and high blood pressure.
The Dietary Approaches to Stop Hypertension (DASH) diet can decrease blood pressure and lower the risk of heart disease.
The DASH diet is rich in fruits, vegetables, low-fat dairy, whole grains, fish, poultry, dry beans, seeds, and nuts. It is low in salt sodium, added sugars, and sweet.
The American Heart Association says people with hypertension should get about 1,500 mg of sodium a day. However, your renal dietitian may have different recommendations depending on your health status.
Nutrition for Cholesterol
Nutrition can play a large role in lowering cholesterol. One thing you can do is start reading food labels. Foods with saturated fat turn into cholesterol when digested in the body. Look for foods that are low in saturated fat. Limit foods made with
- Coconut oil
- Palm kernel oil
- Palm oil
- Lard
- Shortening
- Bacon fat
- Cocoa butter
- Butter
- Margarine
Alcohol can increase cholesterol levels so stick to just one drink a day. Unless your physician says otherwise.
Increase your intake of fiber. Try to get at least 25 to 35 grams of fiber a day. Fiber can be found in fruits, vegetables, nuts, seeds, beans, and whole grains.
Swap fatty animal proteins for lean meats, poultry, and fish. Don’t fry your food. Instead steam, broil, roast, and bake them to lower the fat content.
Nutrition for Diabetes
When you have both diabetes and kidney disease you need to manage not only your blood sugar levels but also the level of nutrients like sodium, potassium, and phosphorus.
Optimizing blood sugar is necessary to manage your diabetics. This starts with your diet.
First, you want to make sure you are not getting too much sugar. Aim to have less than 10% of your calories come from added sugar.
This means if you are consuming 1,800 calories a day you want to get less than 180 calories from added sugar.
Secondly, carbohydrate intake should be monitored. This will ensure you are not getting too many or too little carbs. It will also improve blood sugar regulation.
Normally people with diabetes should get about half of their calories from carbs. So if you have a 1,800 calorie diet you should eat about 800 to 900 calories from carbohydrates.
Carbohydrates have 4 calories per gram. So that gives you a total of 200 to 225 grams of carbs per day.
Another way to keep blood sugar levels stable throughout the day is by eating the same amount of carbs at each meal. If you are someone who takes insulin this may not be necessary since your insulin will match the carbs you eat.
The type of carb you consume also counts. You want to limit your intake of refined carbs. This means fewer cookies, candies, cakes, pastries, white pasta, bread, and other refined foods. Instead, increase your intake of whole vegetables and fruits. These foods contain fiber which is known to regulate blood sugar.
When you have both CKD and diabetes you will also need to monitor your sodium, potassium, and phosphorus levels. Learn more about the renal diabetic diet here.
Nutrition for Diabetes: Sodium, Potassium, and Phosphorus Recommendations
Sodium recommendations are about 2,300 mg per day with ⅓ of it at each meal. If you have hypertension your intake should be around 1,500 mg per day.
Depending on your potassium levels you may need to monitor this mineral. Too much or too little can be dangerous for your health. Your healthcare team can tell you if you need to cut back on this nutrient.
People with poor renal function need to monitor phosphorus levels. If your kidneys are not clearing phosphorus from the body you may need to limit this in the diet. See what your renal dietitian says about your phosphorus intake.
(See what you should avoid when you have sodium, potassium, and phosphorus restrictions at the food list below).
Overall, making healthy food choices, understanding portion sizes, and learning the best time to eat will help manage your blood sugar and prevent your diabetes from worsening.
This means cutting back on processed and sugary foods and drinks. Drinking more water and eating more fresh vegetables, fruit, and unprocessed whole grains.

Nutrition for Anemia
Many kidney patients do not get adequate treatment for anemia. If you have symptoms of this condition it is imperative to correct this deficiency.
Nutrition interventions for anemia include getting more iron, folate, and vitamin B12 rich foods in the diet. These include:
- Leafy green vegetables
- Eggs
- Fish
- Liver
Sometimes iron from food intake can not be enough. Some people may need to take an iron supplement to overcome anemia, such as iron water.
Be sure to discuss this with your healthcare team before starting any iron supplements.
Nutrition for Bone Disorders
Stage 3 of CKD can result in high bone turnover conditions. Treatment involves controlling phosphate, calcium, vitamin D, and parathyroid hormone levels.
Potential nutritional interventions involve:
- Avoiding phosphorus additives in foods
- Limiting high-phosphorus foods that are highly absorbed
- Phosphate binders
- Increase calcium intake with foods and supplements
- Vitamin D rich foods and supplements
Restricting Intake of Phosphorus-Rich Foods
One way to lower phosphorus and increase calcium levels is to reduce dietary intake of phosphorus. Processed and packaged foods often have phosphorus added as a preservative.
If you see any foods with the words “PHOS” steer clear of them. Some foods and drinks are also naturally high in phosphorus, but research shows that even foods naturally higher in phosphorus may not be absorbed well.
(See below for a list of high phosphorus foods to avoid.)
Phosphate Binders
Phosphate binders may also be prescribed if someone’s eGFR is below 50 mL/min. Increasing calcium and vitamin D levels can balance mineral levels. This will improve bone health.
Depending on your levels you may be told to supplement vitamin D and calcium.
Read more about phosphorus binders here.
Increase Calcium Intake with Food and Supplements
Calcium levels should not be too high or too low. When calcium levels drop, PTH will take calcium from the bones. Excess calcium will prevent our body from using vitamin D.
Both processes can leave the bones weak and increase the risk of poor bone health.
One way to prevent this is to increase the calcium in the diet. The health of your kidneys will determine your calcium needs.
Foods high in calcium include:
Many calcium foods are often high in phosphorus. This means if you have a phosphorus restriction you may have to limit your intake of these foods.
Vitamin D Rich Foods and Supplements
Adequate vitamin D is also needed to prevent bone disorders.
The best food sources include:
- Trout
- Salmon
- Tuna
- Mackerel
- Fish liver oil
Mushrooms, beef, liver, cheese, and egg yolks also have some vitamin D.
Depending on your dietary restrictions the intake of some of these foods should be limited.
If you cannot get enough calcium or vitamin D through diet you may need to take a supplement.
Be to ask your dietitian and doctor about phosphate binders, calcium, or vitamin D supplements before taking them.
Nutrition for Nerve Damage and Neurological Problems
Inflammation from PTH, high blood sugar, and AGE’s can cause nerve damage. Eating a diet rich in fresh vegetables and fruits can prevent this.
Those with diabetic CKD regulating blood sugar levels can also prevent the progression of autonomic and peripheral neuropathy.
Diet changes that can improve autonomic neuropathy include an increase in fiber and fluids. Be sure to ask your renal dietitian if you have any fluid restrictions.
Regulating potassium levels also helped prevent peripheral nerve damage.
High potassium levels may also be the cause of uremic neuropathy. It impairs nerve function.
Vitamin B12 deficiency is associated with some cognitive impairment in CKD. Increasing the level of this nutrient may help improve brain function.
Foods rich in B12 include:
- Fish
- Meat
- Poultry
- Eggs
- Dairy products
- Fortified nutritional yeast
Depending on your dietary needs your renal dietitian may recommend a B12 supplement to increase levels.
Nutrition for Uremia
Nutrition for reducing uremia includes improving iron and calcium levels while managing phosphorus, potassium, and sodium intake.
The addition of iron-rich foods like leafy greens and liver will correct iron deficiency. A supplement may be needed.
Be sure to ask your renal RD before starting iron pills.
Calcium and phosphorus levels can be regulated by limiting foods high in phosphorus and increasing calcium-rich foods that are low in phosphorus.
A phosphate binder, vitamin D, or calcium supplement may be needed depending on your nutrient status. As always do not supplement without getting advice from your healthcare team.
Sodium intake should be approximately 2,000 milligrams per day.
Potassium intake will depend more heavily on your lab results, and can range anywhere from 2,000 to 3,000 milligrams to unlimited. Some kidney patients may require potassium supplements to keep levels in range.
Phosphorus intake may need to be limited to approximately 2,000 milligrams per day from natural sources.
Protein intake should also be limited in people with uremia. Recommendations are between 0.8 and 1 grams of protein per kilogram of weight.
This means if you weigh 150 lbs you should be getting between 54 and 67 grams of protein a day.
It’s important to review your protein intake and goals with a dietitian to ensure malnutrition or other kidney complications do not occur from too much or too little protein.
If someone has advanced uremia or malnutrition a low protein diet can cause more damage and increase the risk of needing dialysis.
Nutrition for Electrolyte Disorders (Salt and Water Retention)
The key to improving electrolyte disorders is to regulate sodium, potassium, and phosphorus levels.
Reducing sodium intake can reduce water retention and edema. This means using less salt in the diet.
Ways to lower salt in the diet include:
- Eating more fresh fruits and vegetables
- Use fresh cuts of beef, chicken or pork contain natural sodium
- Canned and frozen fruits are also low in sodium
- Get “fresh frozen” vegetables with no added seasoning or sauces
- Look for products with a low sodium content (less than 130 mg per serving)
- Select spices and seasonings with no sodium
- Look for low sodium options when dining out
You can lower potassium by limiting or avoiding high potassium fruits and vegetables if necessary.
Examples of high potassium fruits and vegetables include:
- Bananas
- Melons
- Oranges
- Potatoes
- Tomatoes
- Dried fruits
- Nuts
- Avocados
- Deep-colored and leafy green vegetables
- Some fruit and vegetable juices
Other foods high in potassium are milk and yogurt, dried beans and peas, most salt substitutes, and protein-rich foods such as meat, poultry, pork, and fish.
Additionally, potassium additives can also increase potassium levels in the blood. Label reading to avoid foods with ingredients including potassium may help control high potassium levels.
Learn more about the low potassium diet here.
Limit or avoid foods high in phosphorus:
- Foods that include phosphorus additives in the ingredient list
- Dairy products (milk, cheese, yogurt, ice cream, and pudding)
- Nuts
- Peanut butter
- Dried beans and peas (kidney beans, split peas, and lentils)
- Cocoa, beer, and dark cola drinks
- Bran breads and bran cereals
However, it’s important to know that where phosphorus is found in your diet is more important than just reducing foods with phosphorus. Learn more about a low phosphorus diet here.
Nutrition for Metabolic Acidosis
One way to tell if you are at risk for metabolic acidosis is by looking at the carbon dioxide in your blood. If your serum bicarbonate levels are below 22 mEq/L you have metabolic acidosis.
Eating foods that produce a high amount of acid can lead to metabolic acidosis. These include:
- Animal proteins
- Sweets
- Some nuts
- Alcohol and beer
Instead, you want to increase your intake of
- Vegetables
- Fruits
- Beans and legumes
- Some nuts
These guidelines are helpful in reducing potential renal acid load, or PRAL, in foods. Learn more about PRAL here.
Nutrition for Weight Maintenance
If you are looking to prevent disease progression you want to maintain a healthy weight. Losing weight may help preserve kidney function. This is because:
- Excess fat crowds the kidneys and compresses them
- A bigger body makes the kidneys work harder
- Inflammation is more likely to be prevalent in those who are obese
Even the loss of just 10 lbs can improve kidney health. It also reduces the risk of complications like hypertension, diabetes, and heart disease.
One way to lose weight is to implement good nutrition. People who have had success with weight loss have incorporated these principles:
- Learn how to make healthier food choices
- Reduce portions
- Reduce intake of unhealthy fats
- Ditch the white carbs and eat more whole grains
- Eat more whole unprocessed fresh fruits and vegetables
- Have lean meats, fish, whole grains, and low-fat dairy
- Learn how to read nutrition labels
- Get more high fiber, low fat, and low sugar foods
- Drink more water
- Limit alcohol intake to 1 or less drink a day
- Keep a food diary
- Make a food shopping list and stick to it
- Don’t go to the food store hungry
Labs to Monitor
In addition to nutrition, certain labs should be monitored when you have stage 3 kidney disease.
Your labs will dictate your dietary needs and help you get the best nutrition possible. The following labs should be monitored by your renal dietitian.
- Renal Function Panel
- Comprehensive Metabolic Panel (CMP)
- Complete Blood Count (CBC)
- Urinalysis
- Iron, Ferritin, and Transferrin Saturation (TSAT)
- Thyroid Panel
Renal Function Panel
The renal function panel is a test used to evaluate kidney function. It is used to help manage CKD and measures compounds in the body including
- Electrolytes
- Minerals
- Proteins
- Glucose (blood sugar)
- Waste products
- Additional calculated values
Read more about the renal function panel here.
Electrolytes
Electrolytes are molecules with an electrical charge. These substances control nerve and muscle function and are vital to life.
They also are needed to regulate fluid balance which prevents metabolic acidosis. They include:
- Sodium
- Potassium
- Chloride
- Bicarbonate (carbon dioxide)
Minerals
Minerals are needed for energy production, bone growth, and muscle and nerve function. They include phosphorus and calcium.
Phosphorus works as a buffer to maintain acid-base balance.
Calcium is one of the most important minerals in the body. It also helps to regulate blood clotting and keep a steady heartbeat.
Protein
Protein levels are measured by albumin. It makes up about 60% of the protein in the blood.
Albumin is responsible to keep fluid in the blood vessels and regulate blood pressure. It also helps move hormones, vitamins, drugs, and electrolytes, and minerals through the body.
Waste Products
Waste products will tell how well the kidney is functioning. These include urea or blood urea nitrogen (BUN) and creatinine.
BUN is a nitrogen-containing waste product that is produced when protein is digested. The liver releases it into the blood and then it is moved to the kidneys.
The kidneys will filter it out to be excreted in the urine. High BUN levels can indicate poor kidney function.
Creatinine is a waste product produced by the muscles. It is sent to the kidneys where almost all of it is eliminated. High levels of this substance can show there is kidney dysfunction.
Glucose (Blood Sugar)
Glucose is what gives the body energy. The blood should contain a consistent amount of glucose that is ready for the body to use.
The urine may also be tested for glucose. This test indicates if someone has diabetes.
If you’re concerned about your blood sugar ask your doctor what your level should be. Blood sugar targets vary from person to person.
In general, it should be:
- Before meals: 90-130 mg/dL
- Two hours after the start of a meal: below 180 mg/dL
To get an average of blood sugar often the healthcare team will look at your hemoglobin A1C.
This test is an average of 3 months of blood sugar levels. Having an A1C of 7% is recommended for those with kidney issues.
Additional Calculated Values
There may also be three additional calculated values that show up on a renal panel. They include BUN/creatinine ratio, estimated glomerular filtration rate (eGFR), and the anion gap.
The BUN/creatinine ratio is the comparison of urea to creatinine in the blood. High levels mean that the kidneys are not functioning well.
The estimated glomerular filtration rate (eGFR) is an assessment of how well the kidneys are filtering the blood per minute. It is based on creatinine levels. This also takes into account someone’s age, gender, race, and sometimes height, and weight.
The anion gap is a value that looks at the difference between measured and unmeasured electrolytes of fluid in the blood.
When the kidneys are not working there will be a dilution of sodium and chloride. When someone is dehydrated potassium, sodium, and chloride levels will be elevated.
Comprehensive Metabolic Panel (CMP)
The comprehensive metabolic panel (CMP) looks at 14 different substances in your blood. It gives insight into how well the body is performing.
A CMP has the tests found in the renal panel with the addition of the following:
- Total Protein
- Liver Enzymes and Bilirubin
- Cholesterol levels
Total Protein
Total protein is how much protein is in the blood.
Liver Enzymes and Bilirubin
Liver enzyme function tests tell how well the liver is working. They include:
- Alkaline phosphatase (ALP)
- Alanine transaminase (ALT)
- Aspartate aminotransferase (AST)
High levels of ALP could mean liver damage.
When AST is high it can indicate heart problems, pancreatitis, and inflammation of the liver or disease.
Elevation of ALT enzymes can occur before symptoms start. These enzymes also indicate damage and disease.
Bilirubin is made by the liver when food is digested. High levels in the blood indicate possible liver damage.
Medications, certain foods, supplements, and strenuous exercise may also affect liver function. So elevated bilirubin and liver enzyme levels do not always mean there is a problem.
Be sure to ask your doctor if you have any concerns.
Cholesterol
Cholesterol is a type of fat in the blood. It is made by the body and also obtained from food.
Testing cholesterol will help determine if you have blood vessel disease which is common among people with CKD.
There are three parts of cholesterol. They include:
- LDL the “bad” cholesterol
- HDL the “good” cholesterol
- Triglycerides
The total cholesterol is also measured. This is the sum of the good and bad cholesterol.
Healthy cholesterol levels are in the table below.
| Cholesterol Types in Lab Testing | Healthy Levels (mg/dL) |
|---|---|
| Total Cholesterol | < 200 |
| HDL (high-density lipoprotein) | >/= 40 |
| LDL (low-density lipoprotein) | < 100 |
| Triglycerides | < 150 |
Talk to your doctor about any questions you have about your cholesterol levels.
Complete Blood Count (CBC) Panel
Complete Blood Count or (CBC) is a blood test that looks at the health of your blood. It includes the following tests:
- Red blood cells
- White blood cells
- Platelets
- Hemoglobin
- Hematocrit
Red blood cells carry oxygen from your lungs to the rest of your body. If this level is low it could indicate anemia, iron deficiency, or heart disease.
White blood cells (WBC) help fight infection. There are five types of white blood cells.
The CBC measures the total number of WBC in your blood. If you get a CBD differential test that means that number of each type of these WBC is also measured.
Both low and high WBC counts could mean a potential health condition. However, abnormal levels could also be due to medications, diet, and for women, menstrual cycles.
Platelets are what help stop bleeding. They are responsible for blood clotting.
Hemoglobin is a protein in the RBC that moves oxygen from the lungs to cells in the body. Not enough hemoglobin will lead to anemia.
Levels in healthy people are between 12-15 g/dL for women and 13-17 g/dl for men. If you have CKD these may be lower. Ask your doctor about what is a good level for you.
Hematocrit is how much of your blood is made up of red blood cells. Low levels of hematocrit show there are problems with the kidneys.
Urinalysis
When you have CKD you should routinely test the urine. This will monitor your kidney function as well as any potential complications like diabetes. It looks at the:
- Color
- Appearance (clear or cloudy)
- Odor
- Its acidity (pH level)
- Presence of bacteria and other germs
It will also look to see if it has anything that should not be there. It is tested for substances like blood, protein, glucose, ketones, bilirubin cells, crystals, and casts (tube-shaped proteins).
Iron, Ferritin and Transferrin Saturation (TSAT)
In addition to looking at hemoglobin in the CBC, another way to know if there is enough iron in the body is by looking at the transferrin saturation (TSAT) and ferritin levels.
Ferritin is a protein that stores iron inside your cells. This level will tell you how much iron storage is available. Levels should be at least 100 ng/mL.
Transferrin saturation (TSAT) measures the amount of transferrin in your blood. Transferrin is a protein made by the liver.
When iron stores get low the liver will pump out transferrin to compensate for the low iron. If your TSAT levels fall below 20% you could have low iron.
Thyroid Panel
The thyroid should be monitored annually. A full thyroid panel includes the following tests:
- Thyroid Stimulating Hormone (TSH)
- Free Thyroxine (Free T4)
- Free Triiodothyronine (Free T3)
- Thyroid antibodies
- Reverse Triiodothyronine (rT3)
- Thyroid Ultrasound
- Signs and Symptoms
Thyroid-stimulating hormone (TSH) indicates how much hormone the thyroid gland is making.
A HIGH TSH means the thyroid is not making enough thyroid hormone. This is known as hypothyroidism.
A LOW TSH means the thyroid is making too much hormone. This condition is called hyperthyroidism.
Thyroxine (T4) is the main thyroid hormone in the blood. The free T4 (FT4) test tells how much free T4 is available for cells to use. This level is looked at in conjunction with TSH to see if there is thyroid dysfunction.
Having an elevated TSH and low FT4 means the person has hypothyroidism. A high FT4 and low TSH means there could be hyperthyroidism.
When both TSH and free T4 are low it means there could be something wrong with the pituitary gland.
Free triiodothyronine (free T3) tests are used to monitor thyroid function in conjunction with TSH. Generally, a high level indicates hyperthyroidism and a low level will indicate hypothyroidism.
Thyroid antibody tests determine if there is an autoimmune thyroid condition such as Hashimoto’s or Grave’s disease.
They consist of the following:
- Thyroid peroxidase (TPO) antibodies
- Thyroglobulin antibody (TG) antibodies
- Thyroid-stimulating immunoglobulin (TSI) Antibodies
- Thyroid binding inhibitory immunoglobulin (TBII) Antibodies
Reverse Triiodothyronine (rT3) is secreted in small amounts by the thyroid. Its presence reflects how well T4 is being used.
rT3 can be useful for knowing if there is thyroid disease if someone is experiencing symptoms but their free T3 is normal. Certain medications may elevate rT3 so ask your healthcare provider about your results.
Thyroid ultrasound can indicate thyroid problems even when blood work looks normal.
Signs and Symptoms to Include in a Thyroid Panel
There are many signs and symptoms of thyroid dysfunction.
Signs of hypothyroidism include:
- Fatigue
- Feeling cold all the time
- Constipation
- Muscle weakness
- Weight gain
- Joint or muscle pain
- Anxiety
- Depression
- Brain fog
- Dry skin
- Hair loss
- Slowed heart rate
- Less sweating than usual
- A puffy face
- A hoarse voice
- Women will experience heavy periods
- High LDL cholesterol
People with hyperthyroid conditions may experience the following:
- Weight loss
- Increased appetite
- Rapid or irregular heartbeat
- Nervousness, anxiety
- Irritability
- Trouble sleeping
- Trembling in your hands and fingers
- Increased sweating
- Feeling hot
- Muscle weakness
- Diarrhea
- Lighter periods (women only)
- Red, irritated or bulging eyes
- Weakened bones
Some people experience no symptoms at all so a blood test and possible ultrasound will give a clear picture of thyroid health.
Nutrients to Monitor
During stage 3 kidney disease you want to be sure to monitor certain nutrients in the body. This will tell you how well your kidneys are functioning.
This will also determine if you need any restrictions in your diet. Typical nutrients to monitor include the following:
- Sodium
- Calcium
- Phosphorus
- Potassium
- Magnesium
- Iron
- Fluid
Sodium
During CKD, sodium levels should be monitored. Normal sodium levels are between 135 to 145 milliequivalents/liter (mEq/L).
Too much or too little of this nutrient can cause hyponatremia and hypernatremia:
- Hyponatremia: sodium levels below 135 mEq/L
- Hypernatremia: sodium above 145 mEq/L
Calcium
A calcium blood test measures the calcium in your blood. Most of the calcium is stored in your bones with about 1% remaining in your blood.
A normal range of calcium is between 8.5 to 10.5 mg/dL (4.3 to 5.3 mEq/L or 2.2 to 2.7 mmol/L).
This may vary by lab up to 0.5 mg/dl. Be sure to ask your healthcare provider what are acceptable calcium levels.
Phosphorus
As kidney function declines, phosphorus will begin to build up in the blood. So it is important to monitor your phosphorus levels.
A normal phosphorus level is between 2.5 to 4.5 mg/dL.
Potassium
Too much or too little potassium can be harmful to the body. You may need to limit the amount of potassium depending on your blood levels.
Potassium levels range from safe to dangerous. They are as follows:
- Safe zone: 3.5 – 5.0 mg/dL
- Caution zone: 5.1- 6.0 mg/dL
- Danger zone: higher than 6.0 mg/dL
Magnesium
Magnesium levels are controlled by the kidneys. During CKD magnesium can build up in the blood.
A normal level is between 0.75 and 0.95 millimoles (mmol)/L.
Iron
As noted above iron is a mineral that should be monitored for health status in CKD.
Hemoglobin, ferritin, and transferrin saturation are what indicate iron status.
Fluid
Monitoring fluid levels can tell how well your kidneys are functioning. High levels of water in the body indicate poor kidney function.
Your doctor may order a 24-hour urine collection to measure how much fluid your kidneys are filtering out. Depending on this result, you may require a fluid restriction.
Foods to Avoid with Stage 3 Kidney Disease
Having restrictions and avoiding certain foods during stage 3 kidney disease will salvage kidney function, minimize complications, and prevent progression of the condition.
Foods High in Added Sugar
You want to avoid added sugar in your diet. This means processed sugary junk foods and drinks. Juices can also contain a lot of sugar and should not be consumed.
Avoid Foods High in Sodium
Foods high in salt are no help to kidneys in bad shape. To prevent fluid retention and high blood pressure you should reduce the sodium in your diet.
This can be done by limiting or avoiding:
- Soy sauce
- Liquid aminos
- Teriyaki sauce
- Garlic, onion, or celery salt
- Canned foods and soups
- Frozen dinners unless they say “low sodium”
- Ham, bacon, hot dogs, sausage deli, and other processed meats
- Salted snack foods (chips and crackers)
- Dehydrated soups
- Most restaurant foods
- Takeout foods and fast food that is high in salt
Avoid Calcium-Fortified Foods
Depending on your calcium levels you may need to avoid calcium-fortified foods. These products could increase your serum calcium and hurt your kidney health.
Limit Foods High in Potassium
If you have elevated blood levels of potassium you will need to avoid foods high in potassium.
This means reducing portions or eliminating certain fruits and vegetables:
| High Potassium Fruits | High Potassium Vegetables |
|---|---|
| Avocados Bananas Cantaloupe Dates Nectarines Oranges and orange juice Prunes and prune juice Pumpkin Apricot fresh or dried Dried figs Grapefruit Juice Honeydew Kiwi Mango Papaya Pomegranate and pomegranate Juice Raisins | Artichokes Acorn squash Bamboo Shoots Butternut Squash Beets and beet greens Broccoli Brussels sprouts Chinese Cabbage Hubbard Squash Kohlrabi Okra Parsnips Potatoes Rutabagas Spinach (cooked) Sweet potatoes Swiss chard Tomatoes and tomato juice Vegetable juice White Mushrooms |
Other foods high in potassium include:
- Bran products
- Chocolate
- Granola
- Baked Beans
- Milk
- Molasses
- Refried Beans
- Black Beans
- Nuts
- Seeds
- Peanut Butter
- Dried Beans and Peas
- Yogurt
- Lentils
- Legumes
- Salt Substitutes/Lite Salt
Avoid Foods High in Phosphorus
Phosphorus restrictions are not common in this stage of kidney disease, but if your labs show phosphorus buildup you may need to cut back on foods and drinks high in phosphorus.
Here is a table of different high-phosphorus foods. If you need to reduce phosphorus in your blood, start with the highly-absorbed phosphorus sources.
If your levels continue to stay high, move to the moderately-absorbed phosphorus foods.
Finally, if you have eliminated all of the foods in the first two categories and phosphorus levels are still high, aim to limit intakes of low-absorbed phosphorus foods.
| Highly-absorbed Phosphorus Foods | Bottled beverages with phosphate additives (words with “PHOS” in them) such as pepper-type sodas, dark colas, canned/bottled teas Processed foods Processed meats Cocoa Baked goods |
| Moderately-absorbed Phosphorus Foods (assuming no phosphate additives are included) | Meats Milk Eggs Cheese Custard Ice Cream Pudding Cream Soups Oysters Sardines Beef Liver Chicken liver Fish roe Organ meats Chocolate candy Caramels |
| Low-absorbed Phosphorus Foods | Beans Nuts Legumes Seeds Grains such as oat bran |
Avoid Foods High in Animal Protein
Those with CKD may need to limit or avoid foods that will put a strain on the kidneys and also contribute to metabolic acidosis. This means going on a low-protein diet and limiting or avoiding animal protein.
Eating less animal protein will help maintain kidney health.
Foods high in animal protein include:
- Beef
- Veal
- Lamb
- Pork
- Chicken
- Turkey
- Fish
- Seafood
- Eggs
You can also get specific protein recommendations from your renal dietitian.
Limit Foods High Refined Carbohydrates
Refined carbohydrates will elevate glucose and weaken the kidneys.
Limit these foods to help lower blood sugar:
- Sugar
- White bread
- Pizza dough
- Pasta
- Pastries
- White flour
- White rice
- Sweets
- Desserts
- Breakfast cereals
- Sugary beverages
Avoid Foods High in Unhealthy Fats
Avoid fats that will increase your cholesterol, bad LDL, and risk of heart disease. These include saturated and trans fats. They are found in the following:
- Fatty meats
- Full fat dairy
- Baked goods (cakes, cookies, pies)
- Fried foods
- Shortening
- Margarine
Any food that has the word “hydrogenated” in its ingredient list has trans fat and should not be consumed.
Avoid Alcoholic Beverages
Excess alcohol intake can put a strain on the kidneys, increase blood pressure, and cause weight gain. One drink is any of the following:
- 12 ounces of beer
- 5 ounces of wine
- 1.5 ounces of liquor
Some recommendations say that one drink a day is ok but it depends on your kidney function. Ask your renal dietitian what is right for you.
Learn more about alcohol in the renal diet here.
Foods to Eat with Stage 3 Kidney Disease
You may be left feeling there are a lot of restrictions during stage 3 of CKD. Don’t fret, there is still a lot you can eat during this stage. In this section we break out the foods you should eat when you have stage 3 kidney disease.
These nutrients will help your kidneys thrive. So let’s dive into what foods to incorporate into your diet.
Low Sodium Foods
We know salt can be problematic for weak kidneys. So look for foods that have little to no sodium. These include the following:
- Fruits
- Vegetables
- Frozen fruit with no added dressings or seasoning
- Fresh garlic
- Fresh onion
- Garlic powder
- Onion powder
- Black pepper
- Lemon juice
- Low-sodium/salt-free seasoning blends
- Vinegar
- Homemade or low-sodium sauces and salad dressings
- Dry mustard
- Popcorn (unsalted or low sodium)
- Pretzels (unsalted or low sodium)
- Tortilla or corn chips (unsalted or low sodium)
- Low-salt deli meats without phosphate additives
- Natural cheese (1-2 oz per week)
- Homemade or low-sodium soups
- Canned food with no added salt and no phosphate or potassium preservatives
- Homemade casseroles with no added salt
- Fresh meat (beef, veal, pork, poultry)
- Fish (fresh)
- Eggs
- Rice
- No added sodium pasta
Packaged foods will often have the terms sodium-free, low sodium, very low sodium, reduced sodium, and light in sodium written on them.
| Sodium Free | Very Low Sodium | Low Sodium | Reduced Sodium | Light/Lite Sodium |
| Trivial amount of sodium per serving. | 35 milligrams or less per serving | 140 milligrams or less per serving | 25% less sodium than the original product | 50% less sodium than the original product |
If you see salt listed in the first 5 ingredients it is probably too high in sodium. This is because ingredients are listed by weight.

Low Potassium Foods
Typically stage 3 does not require a potassium restriction. In fact, many stage 3 kidney disease patients may benefit from eating more potassium.
However, if your potassium levels are in-fact high you will need to incorporate these low potassium foods.
| Low Potassium Fruits | Low Potassium Vegetables |
|---|---|
| Apple and apple juice Applesauce Apricot Canned apricots (in juice) Blackberries Blueberries Cauliflower Cherries Cranberries Fruit Cocktail Grapes and grape juice Grapefruit Mandarin Oranges Peaches Pears Pineapple and pineapple juice Plums Raspberries Rhubarb Strawberries Tangerine Watercress Watermelon | Alfalfa sprouts Asparagus Broccoli (raw) Carrots Celery Cucumber Eggplant Fresh corn (½ ear) Frozen corn (½ cup) Green or wax beans Green and red cabbage Green peas Kale Lettuce Mixed Vegetables Onions Parsley Peppers Radish Water chestnuts (canned) Yellow Squash Zucchini Squash |
Other low-potassium foods include:
- Rice
- Noodles
- Pasta
- Cookies
- Angel food cake
- Yellowcake
- Poundcake
- Coffee
- Pies without chocolate or high potassium fruit
- Cookies without nuts or chocolate
- Brewed tea (black, green, herbal)
You can also reduce potassium content by double-boiling foods. For more information about low potassium foods, check out this article.
Low Phosphorus Foods
Typically stage 3 kidney disease does not require a phosphorus restriction. However, phosphorus is important to be aware of as it may cause additional problems and possibly deteriorate some kidney function.
If your phosphorus levels are increasing you will need to limit your phosphorus intake. This means looking for alternative foods that are low in this mineral. They include:
- Rice milk
- Almond milk
- Cottage cheese
- Vegan cheese without phosphate additives
- Sherbet
- Popsicles
- Greek yogurt
- Apples
- Berries
- Grapes
- Carrot sticks
- Cucumber
- Rice cakes
- Pretzels (unsalted or low sodium)
- Popcorn (unsalted or low sodium)
- Crackers (unsalted or low sodium)
- Poundcake
- Sugar cookies
- Chicken
- Turkey
- Fish
- Beef
- Veal
- Eggs
- Lamb
- Pork
Calcium-Rich Foods (Low in Potassium and Phosphorus)
Some people with stage 3 kidney disease need calcium. Unfortunately, some calcium-rich foods are also high in phosphorus and potassium.
If you require calcium but have a potassium and phosphorus restriction you can increase your intake of these foods:
- Kale
- Arugula
- Tofu
Low Protein and Plant Protein Foods
When the kidneys are not working well a high protein may lead to uremia. Large intakes of animal proteins can also increase your chance of metabolic acidosis.
A way to lower your protein intake is by stretching it out. This will extend your protein in recipes so that a small amount will satisfy your needs.
Here are some ways to do this:
- Pump up thinly sliced meats in sandwiches with a lot of veggies
- Make cream soups, rice, and pasta sauces more filling with milk substitutes like canned coconut milk
- Use meat as a side dish or small complement to your meal, rather than the “main event”
- Mix small pieces of meat like kabobs with a lot of veggies like peppers, onions, and mushrooms.
- Use a lot of veggies mixed with grains like rice and pasta and very little meat
- Make a salad with some small pieces of meat and egg
- Decrease the meat in a casserole and add more veggies or whole grains
- Increase your starch and low-protein pasta in soups
- Stronger cheeses can be used in smaller quantities for the same flavor
Another way to limit protein is by going vegetarian or vegan.
Complex Carbs and Foods High In Fiber
Getting more complex carbs will help to slow blood sugar levels. These can be found in vegetables and whole grains. It is recommended to get at least 6 servings of whole grains per day. These include:
- Whole grain pasta
- Brown rice
- Barley
- Quinoa
- Millet
- Couscous
- Amaranth
Getting enough fiber can also help control potassium levels.
Healthy Fat Foods
Our bodies need fat to function properly, but too much of the wrong fat can cause problems for the kidneys. Healthy fats to incorporate into the diet include:
- Monounsaturated fats (MUFAs)
- Polyunsaturated fats (PUFAs)
Monounsaturated fats (MUFAs) are good for you but they should also be eaten in moderation. They help lower the bad LDL cholesterol. This can reduce the risk of cardiovascular disease. Good sources for MUFAs are
- Olive oil
- Canola oil
- Peanut oil
- Sunflower oil
- Sesame oil
- Avocados
- Nuts
- Seeds
- Peanut butter
Polyunsaturated fats (PUFAs) are also good for cholesterol and lowering heart disease risk. There are two types of PUFAs: omega-6 and omega-3. These are not made by the body and must be obtained from the diet. Sources of PUFAs include:
- Soybean oil
- Corn oil
- Safflower oil
- Some nuts and seeds
- Salmon
- Mackerel
- Herring and
- Trout.
However, depending on your dietary restrictions you may not be able to consume some of these foods. It is best to talk with your renal RD about where to get your fat in the diet.
Stage 3 Renal Diet Menu Plan
If you’re curious about what foods to incorporate into your diet to help kidney health here is a sample stage 3 renal diet menu plan.
| Monday | Tuesday | Wednesday | Thursday | Friday | Saturday | |
| Breakfast | Orange Immunity Booster Smoothie | Orange Immunity Booster Smoothie | Sweet Cherry Steel Cut Oats | Sweet Cherry Steel Cut Oats (leftovers) | Sweet Cherry Steel Cut Oats (leftovers) | Sweet Cherry Steel Cut Oats (leftovers) |
| Lunch | Chickpea Waldorf Salad | Sweet Potato & Black Bean Salad (leftovers) | Chickpea Waldorf Salad (leftovers) | Sweet Potato & Black Bean Salad (leftovers) | Creamy Edamame & Mushroom Pasta (leftovers) | Cream of Celery & Asparagus Soup (leftovers) |
| Snack | Grapes & Almonds | Grapes & Almonds | Brown Rice Chips w/ Salsa | Brown Rice Chips w/ Salsa | Banana with Peanut Butter | Banana with Peanut Butter |
| Dinner | Sweet Potato & Black Bean Salad | Chickpea Waldorf Salad (leftovers) | Cream of Celery & Asparagus Soup | Creamy Edamame & Mushroom Pasta | Swiss Chard, Lentil & Rice Bowl | Swiss Chard, Lentil & Rice Bowl (leftovers) |
| Snack | Brown Rice Chips w/ Salsa | Brown Rice Chips w/ Salsa | Chocolate Almond Butter Pudding | Chocolate Almond Butter Pudding (leftovers) | Chocolate Almond Butter Pudding (leftovers) | Grapes & Almonds |
Interested in getting the recipes, grocery list, and nutrition info for this sample meal plan? Get it here!
Please know that this is only a sample and there is no one right eating plan for everyone. Kidney health, pre-existing conditions, and the levels of protein, sodium, potassium, phosphorus, and calcium in the blood will determine what type of diet you need.
You should meet regularly with a renal dietitian so you can get a personalized meal plan that is tailored specifically to improve your health.
Does Stage 3 Kidney Disease Require Dialysis?
Stage 3 kidney disease does not require dialysis. However, if you’re wondering, does stage 3 kidney disease always progress to needing dialysis? The answer varies depending on how well you’re taking care of yourself.
According to research, stage 3 kidney disease can progress to stage 4. Having renal failure and needing dialysis is rare but is still possible for people with stage 3 kidney disease. Most cases of ESRD were specifically among those with stage 3-B.
If you are worried about disease progression and dialysis the best thing you can do is to adhere to the medical and nutritional recommendations above. These will help to preserve kidney function and stop you from needing dialysis or a kidney transplant.
If you’re curious how to know when you need dialysis you want to look for signs that indicate kidney failure. They include
- Swelling in the extremities (hands, feet, ankles)
- Headaches
- Itchy skin
- Fatigue
- Insomnia
- Nausea/vomiting
- No sense of taste
- Loss of appetite
- Unintentional weight loss
- Little or no urine
- Numbness
- Muscle cramps
- Weakness
- Pain
- Stiffness
- Fluid in your joints
- Brain fog
- Confusion
- Poor memory
Life Expectancy for Stage 3 Kidney Disease
When diagnosed and managed, stage 3 kidney disease varies but is longer than later stages of the disease.
It is very likely you can expand your life by stopping this disease from progressing any further. According to a 10-year-study, about half of the participants with stage 3 CKD prevented further damage and did not experience advanced stages of the disease.
Instead of worrying about how long you have to live, you should focus on how to stop this disease from progressing to the point where you’re putting yourself at risk for death. Furthermore, managing co-existing conditions and complications listed above can improve your life expectancy.
Summary
Though you may be suffering from stage 3 kidney disease there is still a lot you can do to preserve your kidney health. Working to protect your kidneys will minimize complications and prevent disease progression. It will also prevent you from needing dialysis or a kidney transplant down the line.
It all starts with taking charge of your nutrition, health, and lifestyle habits. This means using nutrition interventions to lower inflammation and improve existing conditions such as anemia, hypertension, heart disease, and diabetes.
You also need to be an advocate for your health. This can be done by monitoring labs, nutrient levels, and your food intake. It all starts with having an eating plan that gives you the right amount of protein, calories, vitamins, and minerals.
Avoid foods that can make your condition worse and focus on foods that will give you the right balance of nutrients to help your body thrive. If you’re wondering what is right for you, the best thing to do is work with a renal dietitian to get an individualized nutrition plan that will improve your health.
Jen Hernandez is a registered dietitian, board-certified specialist in renal nutrition, and author of Plant-Powered Kidney Nutrition: Proven Methods and Easy Recipes to Support Your Kidney Health (available on Amazon). She has nearly a decade of experience with kidney disease patients in all stages - from stage 1 through kidney transplant. Jen writes on the blog of Plant-Powered Kidneys to help reach and teach more kidney patients about how they can enjoy more foods in a plant-based diet while protecting kidney health.




Hi Jen, I’m diabetic doing dialysis every other day and just had open heart surgery in March. I would like to know which brand of protein powder is a good choice. Sometimes I need something fast and easy as a option.
Hi Loretta! I totally get it- easy options are very helpful to keep on hand! I’m a big fan of Orgain brand for powders and bars (not the ready-to-drink shakes.. they have added PHOSphates). Check with your dialysis dietitian as well for personalized recommendations.
Jen, I am stage 3A n I thank you for providing this information as it is very helpful.
I’m so glad you’ve found it helpful, Deborah!
Informative guide.
Thank you, Gwendolyn!
Hello Jen,
My boyfriend 3 months ago has been diagnosed as being 3B. He is 59 yrs old. We are so confused with what is good to eat. He has high blood pressure, high cholesterol and gout and is on medication for all.
He currently has lower back pain from his kidneys but the big change this weekend was terrible headache and upper back/shoulder pain. He reached out to his primary care Dr to refer him to a Kidney Dr but was told he isn’t at the point that he needs to see this doctor or even a renal dietitian.
I would love to help him and be his support but I get so confused with everything that I am reading online. Any help and guidance would be greatly appreciated.
Hi Lindy,
Thanks so much for reaching out. I’m sorry to hear about your boyfriend’s health issues. You clearly care so much to be such a great support and advocate for him! I would really encourage pushing for a dietitian. Everyone can use the help of a dietitian in any stage of CKD. And the earlier a dietitian can see him, the better. We have many more opportunities to help the earlier we can address health conditions- especially CKD! Go back to the doctor and stand up for that referral. If you need help finding a dietitian, here’s a link to my page of dietitian resources.
Jen…………How low should your phosphorus level get down to, to stop the itching.
Hi Richard! It may need to be in the 3’s for the itching to stop. I discuss this in a few articles: check out Itching in Kidney Disease, Low Phosphorus Diet, and Phosphorus Binders. I hope this helps!
Thanks so much for your response. Will be glad to see more from u.
Thank you, Felix!
I am so very confused I read some of these papa paragraphs and it says that broccoli is a no no because it’s so high a potassium in Brussels sprouts and then I go down a few more paragraphs and it says that that’s on the list of things you should eat speak what articles does no donita is bad for you the next article says no it’s perfectly fine it’s very very confusing
Whoops! Thanks for catching that, Sally. Broccoli is considered a high potassium food as it has 230 milligrams of potassium per cup of raw. But if you stuck to a 1/2 cup serving, it would be only half of that. Therefore, it would qualify as low potassium in a smaller serving. But you’re right- including it on both lists can be very confusing and that was a mistake.
The big thing about a renal diet is that pretty much anything can fit if you want it to. It comes down to following your own CKD journey and working with a healthcare team that can guide you.
We can’t say everyone should eat this or no one can eat that, because that isn’t true. I know this doesn’t make things much more clear, but know that there are so many opportunities and flexibilities in finding the right CKD diet that works for you and your kidneys. 🙂
Hello Jen,
I have an appointment with one of you this next week on Monday.
I discovered two months ago that I am in Stage 2 in my country, El Salvador. Sadly, I found that my PCP in the US for 24 years never mentioned that my GFR jumped up and down for several years. Why don’t doctors alert us to these things? He always was saying that my menopause was related to my urination. I am 54 with a GFR of 64 in blood, but the 24 urine test shows 75 GFR. So far, all no protein in my urine and phosphorus, sodium, and potassium are still inside the normal ranges. My big surprise was that I was not drinking enough water according to my height, weight, my active life, and I was eating a healthy diet, but it was not friendly for my kidneys!
I have two questions for you.
What is GFR more exact? The one in the blood that is a formula or the 24 hours urine test that I produce?
Do you think that with a friendly kidney diet, I will have my ranges (min and max) of protein, phosphorus, potassium, and sodium that keep my fingers crossed that I will stay in stage 2 for a longer time?
Sorry for the long post. I want to do what it takes to keep my kidneys healthy and see my family for a long time.
Hi Rox,
Thanks for your thoughtful response!
GFR is essentially how much your kidneys are filtering at any point in time. Think of it like if you were to measure how much water is going through a garden hose when it’s turned on. This will change with every test- don’t expect it to be the same number each time. There are a lot of factors to consider when GFR changes.
We have worked with many clients that have retained or improved their kidney function. The likelihood of this happening increases the sooner you do something, so taking care of it at stage 2 is great! Check our success stories – I think you’ll see some motivational reads there. 🙂
Great information! Thank you Jen.
You’re most welcome, Gail! 🙂
Hello, Jen, Is there an ultimate guide for stage 1?
Thank you for providing so much of information at one place.
Hi Praveena! At this time, we do not. We have guides for stage 3, stage 4 and stage 5.
Hello, thank you
I have purchased two bags of black beans. The nutrition facts are not the same.
they both list the serving size as 1/4 cup however one is 56g the other 35g
35g @ 80 calories 210mg potassium ~ protein 8g
56g @ 130 cal and 850mg potassium ~ protein 13g
The other items in the list are also off.
Which label do I trust? Target or La Preferida?
Thank you
Hi Michael! Great question. Often, the serving size of these types of food will include specifics like cooked or dry. Check the label to see if there’s more description included with either. A cup of cooked beans is approximately 172 grams – so a 1/4 cup of cooked would come out to about 43 grams. From there, the potassium content is about 152 milligrams and protein content is 4 grams.
Here’s the link to that information: https://fdc.nal.usda.gov/fdc-app.html#/food-details/173735/nutrients
This was so helpful to me. My doctor never explained to me what kidney disease stage 3b is. Thank you!
So happy to hear that, Doris! We’re glad to be a resource for the kidney community. 🙂
My husband is a diabetic who has stage 3a CKD GFR @ 45. The CKD was sudden onset from IV antibiotic treatments of Tobramycin. Question is a year ago he had history of Uric acid kidney stones when he first started eating WFPB. He had to have surgery twice. Urologist put on potassium citrate but then potassium too high so now off. Is he more at risk for calcium oxolate kidney stones? We are trying to follow Dr. Esselstyn reversing heart disease (he also had cardiac tamponade). If his potassium is now 5.0 is it okay to eat the greens or does he still need to be careful about oxolate stones
Hi Terri! Thank you for your comment. Unfortunately, we aren’t able to discuss personal medical and nutritional concerns here. It’s best to discuss your husband’s case in more depth with his medical team. (Something we always encourage is to keep asking questions until you feel comfortable with and understand the answers). Good luck!
I have stage 3 kidney disease my doctor wants an MRI with contrast for another health issue
all i have read is that contrast is not a good idea with stage 3 kidney disease, your thoughts.
As this is a medical question, Paul, we recommend you discuss this further with your healthcare team. We’re all about the food here. 🙂
Hi Jen
I currently take medicine Lamivudine every day. Last three month, I have conducted the blood test, found my GFR is still downing from90 to 70 and creatinine is 1.25.
Based on result, how can I increase GFR, please?
Appreciated your advices.
Best regards,
Ratana
Hi Jen,
Is buckwheat ok for CKD stage 3a?
My potassium is at 3.9, EGFR at 48, protein at 6.2 and been on plant base for 3 weeks.
Thanks
Evelyn
Hi Evelyn,
Thank you for your comment.
In general whole grains like buckwheat are a great way to make a filling meal.
Check out our Renal Diet Grocery List buckwheat is on the list.
Hi Jen,
Thanks for coming up with this page. I believe we can breathe a sigh of relief. My Dr seem so lethargic and dependent of google. I felt hopeless with a GFR of 54 (everything else is normal as seen on my labs) that’s maintained itself for the last year in between tests. That’s good right?
Looking forward to trying your dietary plan and praying that I can get my GFR back up just like Dadvice (and many others) have been able to accomplish.
God bless you for your efforts and showing us an alternative solution to kidney health.
Thank you.
Charles