The renal function panel (aka renal function tests or RFTs) is one of the blood tests your physician will order when you have kidney disease. This test is reviewed by your doctor and team, including your renal dietitian. Your labs can provide your healthcare providers with details of what is going on inside your body- whether you realize it or not. In this article, we’ll cover exactly what an adult renal function panel includes.
Table of Contents
Preparing for Your Renal Panel
As with most tests, preparation can be a very important part of tests. This includes lab tests.
When Should I Get a Renal Function Panel?
Your provider will determine whether or not you need a renal function panel.
Some of the other health conditions that may result in a physician lab order it include;
- High blood pressure
- High blood sugars or a diagnosis of diabetes
- Cardiovascular disease
- Obesity
- High cholesterol

Additionally, your doctor may order the testing if you have a family history of kidney disease or show signs and symptoms of kidney issues.
Some symptoms can include;
- Swelling around the hands, feet, ankles, or face
- Changes in your urine like decreased frequency, presence of foam or blood
- Pain to your mid-lower back where the kidneys are located
How Long Does it Take to Get the Results?
Generally, renal lab test results are reported within 24-48 hours.
Many doctors, however, will require “signing off” the results prior to passing them on to the patient.
This means it may take more than 1 business day for you to get your test results.
What Type of Sample is Required?
A renal function panel requires a blood sample. This blood sample is taken from a vein in your arm by a phlebotomist.
This may be done in your doctors office or at a separate lab location.
Do I Need to Fast Beforehand?
Your doctor will instruct you on whether or not you need to fast.
Fasting is generally not required for the renal function panel. However, it may be ordered with other lab testing that could require fasting.
To fast before a blood test, do not eat any food for 8 to 12 hours before the appointment time.
What about drinking water?
It’s important to still drink plenty of water before as dehydration can negatively affect your renal function test results.
However, drinking an excessive amount of water can also change how the renal function panel looks.
The safest amount of water to drink is enough to stay hydrated and avoid thirst. Be sure to follow your doctor’s order for any fluid restriction during this time as well.
Can Fasting Too Long Affect the Results?
Fasting for an excessive period can affect your results by causing a lower glucose level.
If you don’t have enough water, that can also cause abnormalities in your eGFR, sodium, and chloride levels.
Renal Function Panel Test Frequency
Renal function panels may be ordered anywhere from every month to annually (once per year). The timing will be based on your nephrologist or physician’s orders.
You may have a had a renal panel or renal function panel before if you have told your doctor about a family history of kidney disease, or you are already aware of your own diagnosis of kidney disease.
Many doctors are open to having more frequent renal function panel labs drawn when requested.
However, be prepared to put in work if you want to get your renal function panel drawn more frequently.
Renal Function Panel vs. BMP
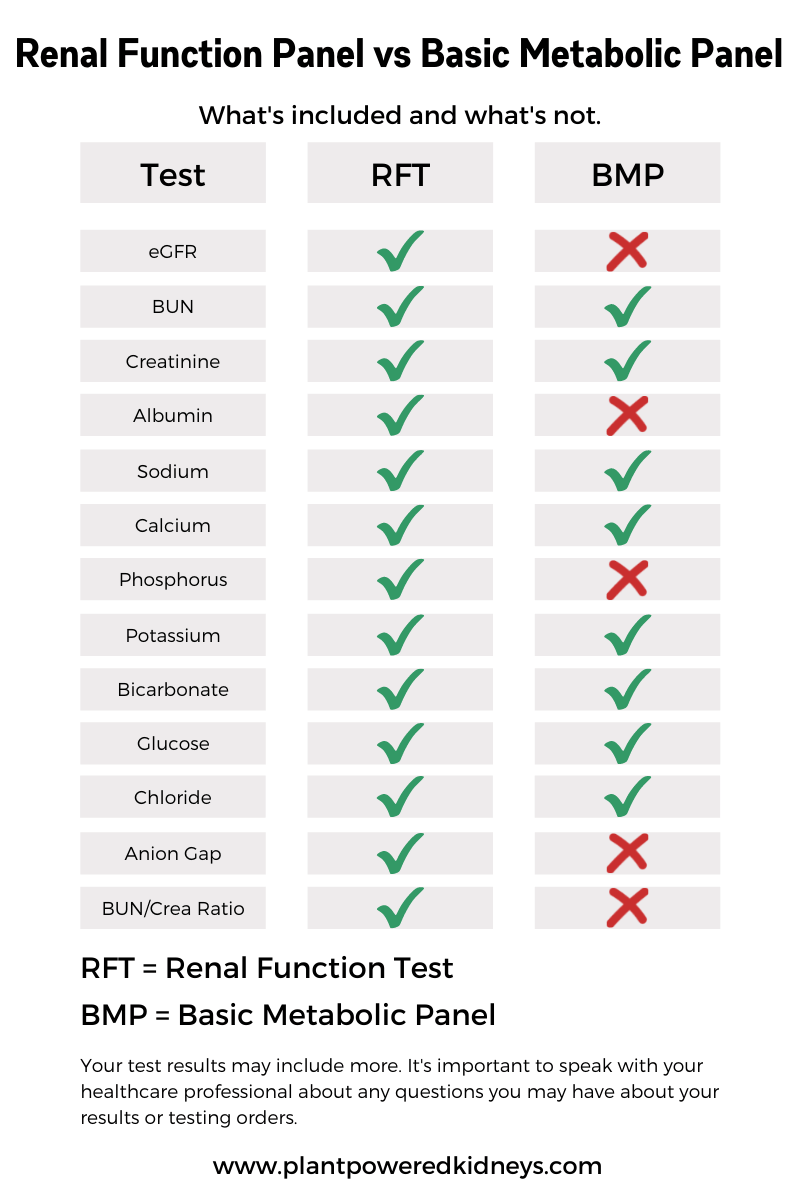
While similar, a renal function panel is slightly different from a basic metabolic panel, or BMP.
Below is a comparison chart between the two tests.
Renal Function Panel Test Details
Next, we’ll cover the different common lab values included in a renal function panel.
We will include standard ranges for the results. However, it’s important to discuss labs with your own healthcare provider as every lab and doctor’s office can have slightly different ranges.
Also, it’s important to note that some people may have “normal” ranges that are outside the standard ranges. This will come from your doctor.
Waste Products
The first group of renal function panel results include waste products.
These are the wastes that are normally produced in the body and eliminated by the kidneys.
Therefore, they are included in this panel to assess how well the kidneys are managing these waste products.
Blood Urea Nitrogen
Blood urea nitrogen, otherwise known as urea nitrogen or BUN, is a measurement of protein breakdown and muscle maintenance in the body.
BUN is generally below 20 mg/dL but will typically rise when there is kidney damage present.
This is because the kidneys are unable to keep up with eliminating excessive waste.
BUN may trend around 75 mg/dL and even higher when on dialysis.
A low-protein diet may help lower BUN for those not on dialysis. However, if done improperly it can increase the risk of protein-energy wasting and malnutrition.
This can then increase inflammation and potentially increase kidney damage. Ketoanalogues can also help lower BUN levels when paired with a low-protein diet.

Creatinine
Creatinine is a waste product from normal muscle metabolism and breakdown. Additionally, creatinine can vary for many reasons. These reasons include gender, age, and activity level.
A normal serum creatinine level is between 0.6 – 1.2 mg/dL for males and 0.5 – 1.1 mg/dL for females.
Eating a high protein diet may impact creatinine levels.
One study found that eating meat prior to a blood draw for creatinine testing, creatinine was falsely higher.
Creatinine will generally go up as kidney function goes down. This is because with CKD, the kidneys aren’t eliminating waste from the body.
Creatinine levels measured in chronic kidney disease can range anywhere from 2.0-15.0 mg/dL depending on the stage and other health conditions.
Finding other culprits that impact your kidney health may help to lower or stabilize creatinine levels. This can come from dietary changes that help promote a healthy kidney.
Protein in the Blood
Albumin
Albumin is a protein that is made in the liver. The serum albumin is a measurement of how much albumin is in the blood.
It was previously thought was that albumin would indicate how much protein you are eating. We now know that it is much more than just that.
Normal albumin will range from about 3.4 – 5.0 g/dL.
As it can signal problems with inflammation, albumin will go down when there is more inflammation.
If you’ve been hospitalized and have access to your hospital labs, take a look at your albumin before, during, and after your hospitalization.
You may see your albumin is on the lower end, or below normal range.
When a person is hospitalized, they can have high inflammation in the body. Once they get better, the albumin can increase. This can show the healing process using the protein albumin.
Evidence shows that following a low-protein diet does not significantly alter albumin levels.
Electrolytes
One of the kidneys’ jobs is to balance electrolytes. This is why these electrolytes are included in the renal function panel.
Sodium
Sodium is the most common particle in our blood outside of our cells. It helps with muscle function, acid-base balance, cellular balance, and osmotic pressure of body fluids.
Many associate sodium levels with the amount of salt in the diet. However, it is more than just that.
Your blood test result is not a reliable measurement of your sodium intake. It is a better measurement for your fluid balance.
The blood serum sodium levels are typically between 135 – 145 mEq/L.
If you experience edema or swelling of extremities with excessive fluids, you may see a slightly lower sodium level.
Additionally, sodium levels may also be falsely low if you drink a lot of water right before your blood draw.
A sodium level above the normal range may be a sign of dehydration.
It’s been thought before that if your sodium is out of range that you should eat more/less salt. That may not necessarily be the case and may cause more issues.
Consult with a registered dietitian to help assess all factors that may be causing an abnormal sodium level before making drastic diet changes.
Working with a dietitian will help save you time and guesswork.
Potassium
Potassium is the third most abundant mineral in our bodies. It acts as an electrolyte and helps with nerve conductivity, muscle contraction, and fluid balance.
The potassium level found in your renal function panel or basic metabolic panel is generally between 3.5 – 5.0 mEq/L.
High- and low-potassium values should be reviewed promptly with your physician and healthcare team as potassium plays an important role in our heart function.
If your potassium levels are consistently above 5.0, you may need to follow a low-potassium diet.
Potassium levels that are out of range are generally a critical concern. Your healthcare provider may follow-up with you quickly and have your levels re-checked.
It’s very important to follow your providers directions when reviewing and managing your potassium levels.
Bicarbonate
Your serum bicarbonate (or carbon dioxide or CO2) is related to the acid-base balance, or pH levels, of your body.
With kidney issues, the bicarbonate levels tend to decline. As a result, the body then leans towards a more acidic state.
Normal bicarbonate levels in the blood are approximately 23 – 28 mEq/L.
Low bicarbonate levels have been associated with an increased risk of kidney problems. This is caused by metabolic acidosis, a common outcome of prolonged kidney damage.
By paying attention to the potential renal acid load (or PRAL) in your diet, you may be able to keep your kidney function with healthy diet changes.
Chloride
Chloride is a negatively charged electrolyte. It helps to balance your fluids as well as your acid-base balance.
The blood serum levels of chloride are generally between 98 – 106 mEq/L.
A low level of chloride may indicate overhydration or be a result of excessive vomiting.
Low chloride can also be due to other health issues like diabetic ketoacidosis, aldosterone deficiency, Addison disease, emphysema, or chronic lung diseases.
High levels of chloride can indicate dehydration. However, it can also indicate health issues including kidney disease due to the imbalance of the acid-base balance that the kidney helps with.
Minerals
Just like electrolytes, the kidneys also manage mineral levels.
Here are some minerals that your doctor may include in your renal function panel.
Phosphorus
Phosphorus is another mineral found in our body. It’s actually the second highest in quantity, behind calcium.
Phosphorus does plenty of things to help keep us healthy, such as;
- manage how your body uses energy
- build strong bones and teeth
- regulate vitamin use
- help with muscle contraction (including our heart)
Blood serum levels of phosphorus should generally be approximately 2.5 – 4.5 mg/dL.
However, ranges may differ depending on the individual.
Even though there is some “forgiveness” with slightly higher phosphorus levels, the Kidney Disease International Outcomes Guidelines (KDIGO) strive for phosphorus within the normal range to prevent increased risk of death.
It may be important to follow a low phosphorus diet if phosphorus is above 4.5.
Phosphorus binders may also be prescribed in some cases to help lower and control phosphorus.
Calcium
Calcium is the number one mineral stored in our body. It helps with many things including bone health and muscle contraction.
General calcium levels are between 8.7 – 10.5 mg/dL.
As our kidneys help regulate our bone health, calcium becomes an important value to monitor with kidney disease.
With many people with CKD, calcium can trend out of range. Calcium can either go above the healthy range or below.
This often leads to either including or avoiding calcium supplements, depending on your labs and other health conditions.
Never take calcium supplements without first discussing them with your nephrologist.
Too much calcium can lead to calcification in your soft tissues. As a result, it can lead to an increased risk of heart attack and stroke.
Energy
You may not realize it, but our energy levels and balance are also important with kidney health.
Glucose
Glucose is considered the primary source of energy for our body. It is taken from the blood into the cells with the help of insulin.
It’s important the level of glucose in our body doesn’t get too low or too high.
The normal range for glucose is broken down into two categories: fasting or non-fasting.
Non-fasting just means you ate something in the hours or day before your renal panel.
Again, it’s important to find out if you should be fasting or not. A renal function panel alone does not generally require fasting.
Fasting glucose is between 70 – 100 mg/dL. For non-fasting glucose, it’s normal to have a level at or below 200 mg/dL.
If you have diabetes, your glucose goals may be different than these reference ranges.
Learn more about the renal diabetic diet here.

Kidney Function Tests and Calculations
Next, we’ll cover some of the other calculations and tests that may be included in the renal function panel.
Glomerular Filtration Rate
The glomerular filtration rate, or GFR, is a measurement of your kidney function of blood filtration.
This is a calculation based on your gender, age, size, and creatinine in your blood.
This is one of the most common tests to assess your kidney function.
A normal GFR is above 90. Some lab reports will look for a GFR of at least 60, as the function will naturally decline as we age.
GFR is associated with stages of kidney disease. Kidney failure is associated with a GFR below 15. However, not just one low value will be enough to confirm kidney issues.
A low GFR for three months can indicate kidney disease along with a diagnosis from a physician.
Urea-to-Creatinine Ratio
Also known as the BUN-to-creatinine ratio or BCR, this is a calculator to evaluate waste removal.
The reference range for this ratio is anywhere from 6 – 22.
Since it is a ratio, changes in either Blood Urea Nitrogen or Urea will affect this level.
Increased levels can be caused by congestive heart failure or dehydration.
Decreased levels can be related to liver disease or malnutrition.
Anion Gap
The anion gap is a calculation of your electrolytes: sodium, potassium, chloride, and bicarbonate.
The anion gap calculation is:
[Sodium (mEq/L) + Potassium (mEq/L)] – [Chloride (mEq/L) + Bicarbonate (mEq/L)] = Anion Gap
The reference range for the anion gap is 8 – 16 mEq/L.
The anion gap calculation can be a factor when evaluating for metabolic acidosis for this reason.
However, it is important to look at each electrolyte in the equation when evaluating reasons for high- or low levels.
Renal Function Panel Normal Values Chart
Below is a table of the reference ranges for tests included in the renal function panel. There is also a column for the abbreviations you may see.
Test | Abbreviation | Reference Range |
Sodium | Na | 135 – 145 mEq/L |
Potassium | K | 3.5 – 5.0 mEq/L |
Chloride | Cl | 98 – 106 mEq/L |
Bicarbonate | CO2 | 23 – 28 mEq/L |
Phosphorus | P | 2.5 – 4.5 mg/dL |
Calcium | Ca | 8.7 – 10.5 mg/dL |
Glucose | Glu | 70 – 100 mg/dL fasting OR <200 mg/dL non-fasting |
Blood Urea Nitrogen | BUN | 6 – 20 mg/dL |
Creatinine | Cr | Adult males: 0.6 – 1.2 mg/dLAdult females: 0.5 – 1.1 mg/dL |
Albumin | Alb | 3.4 – 5.0 mg/dL |
Estimated Glomerular Filtration Rate | eGFR or GFR | >60 |
Anion Gap | AG | 8 – 16 mEq/L |
Blood Urea Nitrogen-Creatinine Ratio | BCR | 6 – 22 |
It’s important to know that the reference ranges may be slightly different on your own test results.
Discuss any questions related to your own renal panel results or reference ranges with your physician.
What Other Lab Tests Besides the Renal Panel May Be Needed?
Depending on your own health history, diagnosis, and situation, there can be other types of tests that are done in addition to the renal function test.
Cystatin C
Cystatic C is a protein made in the body and used to assess kidney function. With good kidney function, the level of cystatin C remains balanced.
It’s seen as a better marker for kidney issues compared to creatinine as it is not easily influenced by muscle mass (like creatinine is).
For those with kidney issues, cystatin C can build up.
Many GFR calculators ask for cystatin C levels to confirm the kidney function or stage of CKD.
Cystatin C is not part of the renal panel, but may be ordered by the doctor if labs in the renal panel are abnormal or suggest kidney damage.
Similar to creatinine, cystatin C levels will be different based on age.
The reference range for adults under the age of 50 is between 0.53 – 0.92 mg/L.
For adults over the age of 50, the reference range is between 0.58 – 1.02 mg/L.
Parathyroid Hormone
The parathyroid hormone (PTH) levels are measured because the kidneys directly tell the body how much of the hormone is needed.
PTH is responsible for balancing the calcium and phosphorus levels in our blood and body.
A normal intact PTH (or iPTH) level is between 10 – 65 pg/mL.
When the kidneys aren’t working well, this number tends to increase. This can lead to up to ten times as high as the normal range.
This increase is expected in kidney disease. While it may not return to the normal range, PTH should be monitored and stabilized.
One of the labs that can greatly influence PTH is phosphorus. High phosphorus can cause higher PTH levels.
Many people with high PTH are encouraged to follow a low phosphorus diet and take phosphorus binders as prescribed.
Vitamin D
We get vitamin D is from the sun and our diet. It is activated by our kidneys.
Normal vitamin D levels are at least above 20 ng/mL. Vitamin D toxicity can occur if levels are over 100 ng/mL.
When kidneys aren’t working as well, vitamin D levels tend to decline.
KDIGO guidelines have addressed that vitamin D deficiency is common in CKD. Therefore, many people with kidney disease supplement with vitamin D.
Appropriate dosing is very important. It is unhealthy and dangerous to have high vitamin D levels in the body.
Always consult with your nephrologist and renal dietitian about the amount of vitamin D you should be taking.
Additional Tests for Kidney Health
Your doctor may order additional tests to better assess your kidney health.
Some of the tests can include;
- Hemoglobin A1c for blood sugar control
- Lipid Panel
- Complete Blood Count (CBC)
- Iron Panel
- Thyroid Panel

Other Types of Kidney Tests
Depending on your lab results, your doctor may order additional tests to assess your kidney function.
Ultrasound or CT Scan
You may have an ultrasound or CT scan of your kidneys. This will give the doctor a picture of your kidneys and urinary tract.
It will help show physical signs of kidney problems, such as size, kidney stones, tumors, or other abnormalities.
Biopsy
Your doctor may also want a kidney biopsy. This procedure requires a tiny sample of your kidney tissue.
The sample is studied under a microscope. A kidney biopsoty may not be necessary depending on your labs.
Many doctors will not order a biopsy if other tests have already confirmed a certain diagnosis, or there would be no benefit in the procedure.
Urinalysis
Finally, your doctor may also order a urine test, or urinalysis. This is a test in which you provide a small sample of urine.
The sample is analyzed visually, with a microscope, and with a dipstick.
A urinalysis can check for creatinine clearance, protein leaking, glucose, white blood cells, and crystals among other issues.
After You Get Your Lab Results
As mentioned earlier, there are important steps to cover with your doctor after you receive your renal function panel results.
A Renal Function Panel is Not Diagnostic Itself
Lab results are a snapshot of what is happening at the time of your blood draw. Therefore, one test result cannot provide a diagnosis of CKD.
Your labs will change from result to result.
It’s important to know that just one result that is out of range may not tell much. Getting retested is important to confirm any outlier.
Track the patterns and changes to get a better feel for how your body and kidneys are doing.
Your physician will likely order follow-up labs for confirmation and diagnosis if a lab result is outside of the expected range.
Make a Plan with Your Provider
Review your results and ask as many questions as needed for you to feel comfortable with your results.
You may or may not have all of these labs in your results – your physician will determine which labs are necessary.
Discuss any labs of concern with your doctor, including what should be done to improve them.
This is also a good time to talk about when you’ll be getting labs drawn again.
Learn more about questions to ask your kidney specialist here.
Seek Out Specialists
Depending on your results, you may benefit from a specialist to help you in a certain area.
Registered dietitians help people by providing further explanations of nutrition-related labs and how your diet can impact your health.
Working privately with a dietitian will give you more concrete answers on what your own lab results mean and how your diet can help improve your levels. This isn’t just for dialysis.
Dietitians help all stages of CKD, from all stages to and through kidney transplant.
Summary
A renal function panel is a set of labs that are ordered by your doctor when reviewing your kidney function.
This set of labs will include waste products, electrolytes, and nutrients like protein and glucose. Your lab results will list out your values alongside standard ranges.
If a lab result is outside of the normal range, your physician may order a follow-up lab testing to recheck it. However, some kidney patients may have “normal” levels despite seeming out of range.
When looking at your renal function panel, it’s important to know that it’s a snapshot of your health. Lab tests alone do not provide a diagnosis and cannot tell the whole story.
Speak with your doctor to see if a renal function panel would be helpful for your health goals. While using this article as a reference for the different labs, it’s important to discuss your results with your doctor.
If you are interested in diving deeper into what kidney labs are all about, enroll in Kidney Labs 101, our online and self-paced class that teaches you about how to discuss your labs with your provider and how nutrition can play a role (even when your provider says diet doesn’t matter)! Click here to learn more.

Jen Hernandez is a registered dietitian, board-certified specialist in renal nutrition, and author of Plant-Powered Kidney Nutrition: Proven Methods and Easy Recipes to Support Your Kidney Health (available on Amazon). She has nearly a decade of experience with kidney disease patients in all stages - from stage 1 through kidney transplant. Jen writes on the blog of Plant-Powered Kidneys to help reach and teach more kidney patients about how they can enjoy more foods in a plant-based diet while protecting kidney health.




This information was very helpful. I have high potassium can you give me some information on what to eat. I’m stage 3. With high protein in my urine. I also suffer with constipation. Any tips will be appreciated. Thank you
Hi Gwendolyn! I’m glad the information helped. I’d recommend you check out the article about the Renal Diet Grocery List: A Comprehensive Guide to Get You Started. Also, our Plant-Powered Kidneys course is open for enrollment this week. We start together next week. I highly recommend you check it out!
Pingback: Renal Function Panel Test: Understanding your kidney lab results and what the numbers mean - Healing Gourmet Keto Recipes
Very useful information. Thanks for all you do.
Thank you for your kind words, John!! 🙂
Very useful information. Thanks for all
You’re welcome! 😊
Rising duties and commitments of first-year students nice thanks
You’re welcome! 😊
I WOULD LIKE TO KNOW IF CHIA SEEDS ARE OK CKD STAGE 2 FOR MY FIBER IN MY SMOOTHIE EVERY MORNING WITH ALL FRUITS, OATS, ALMOND MILK. SINCE I STARTED PLANT BASE DIET I LOST 10 LBS. I THINK IM NOT GETTING ENOUGH FOODS IN PER DAY AND WHAT KINDS EACH DAY.
Hi Judith, Thank you for your comment. Chia seeds are great for breakfast for more breakfast ideas click here >>> If your losing weight unintentionally you may want to reach out to your doctor or dietitian. Best of luck on your health journey!
Pingback: Renal Function Panel: Know Your Numbers | Plant-Powered Kidneys – My Blog
Hi Jen thank you for all you’re doing to help us in a Doctor, Pharm and Insurance company lead life now. As you know there are many things we can do that don’t need modern medicine for. I’ll leave that right there. As I’m new at this CKD stuff I think I have a handle on it and actually have my PCP curious how I am doing. I am obese and and medicines they offer are mostly injections. Then I find out my insurance won’t pay for it. I guess they rather pay the high cost of my many Issue it is causing. It’s been a 6 year battle with weight from morbily obese 400lbs in 2018 to now obese 247 At 5’8″. On my own without any diet tricks or flips. IE Atkins, WW, now the keto and others. You have helped me personally to understand a few things on my Journey with Dadvice and here. I just sat in your Anemia class it was wonderful. Goes by way too fast, but not in a bad way. Lots and lots of info. Thanks again Jen I’ll get ya some updates from time to time.
Thank you so much for sharing, Michael. Traditional healthcare can be tricky for sure, and have limitations. However, we love to teach methods that don’t rely (entirely) on healthcare – things we can do at home in our day-to-day life. I’m so happy you enjoyed our anemia class! And yes, please give us an update as you move forward in your kidney health journey.
Hi Jen! As you know, I am a continuing student, and I have seen the heat chart before, but this is the first time I have seen the info on the RFP and the BMP. It is so much easier to read a chart, so thanks for the infographics! It’s very important to know how to interpret test results. I like to take a peek at them before my doctor appt, so I know what to expect! Thank you.
Hi Darlene! I’m so happy to hear this is helping you. You’re doing a great job, keep it up! 💚