When you have kidney disease it’s important to be careful with phosphorus in the diet. This is because eating foods containing this mineral can lead to high phosphorus levels. As a registered dietitian with experience in both the CKD and dialysis worlds, I know phosphorus all too well after teaching it to thousands of kidney patients. In this article, we will discuss why phosphorus is important, how it can be difficult to control in a renal diet, low phosphorus foods, high phosphorus foods, and what to look for when following a low-phosphorus diet.
Table of Contents
What is Phosphorus?
Phosphorus is an organic compound.
It is an essential mineral that exists in two forms: organic phosphorus and inorganic phosphorus.
Organic Phosphorus
Organic phosphorus is phosphorus that occurs naturally in foods.
It also makes up your bones, teeth, DNA, and cell membranes.
This type of phosphorus is poorly absorbed by humans. Humans do not have the digestive capabilities of breaking it down.
Later in this article, we will cover more details about low phosphorus food groups with organic phosphorus.
Inorganic Phosphorus
Inorganic phosphorus is made in a lab. It is added to food as a preservative.
Inorganic phosphorus is more dangerous for people with kidney issues.
This is because inorganic phosphorus is highly digested and absorbed into the blood stream.
Similarly, we will cover inorganic phosphorus food sources later in this article.
Phosphorus Functions
As mentioned, phosphorus is needed for healthy bones, teeth, and other parts of the body.
Other benefits of phosphorus include the following:
- Energy production
- Enzyme activation
- Regulating gene function, including DNA and RNA structures
- Balancing body pH
Additionally, phosphorus regulates vitamin D and parathyroid hormone (PTH) levels.
Both of these are needed for healthy bone growth and maintenance.
Interestingly, phosphorus is also considered a uremic toxin.
A review in 2021 identified the connection between phosphorus and a healthy (or unhealthy) gut.
recommended daily intake of phosphorus
The U.S. Institute of Medicine determined the Estimated Average Requirement (EAR) for adults to be 580 milligrams per day.
The Recommended Dietary Intake (RDI) is 700 milligrams per day for adults.
For pregnant women and children without kidney disease, it’s recommended to consume 1,250 milligrams of phosphorus daily.
While this may seem high, it’s not.
The average American diet has nearly double the required amount of phosphorus.
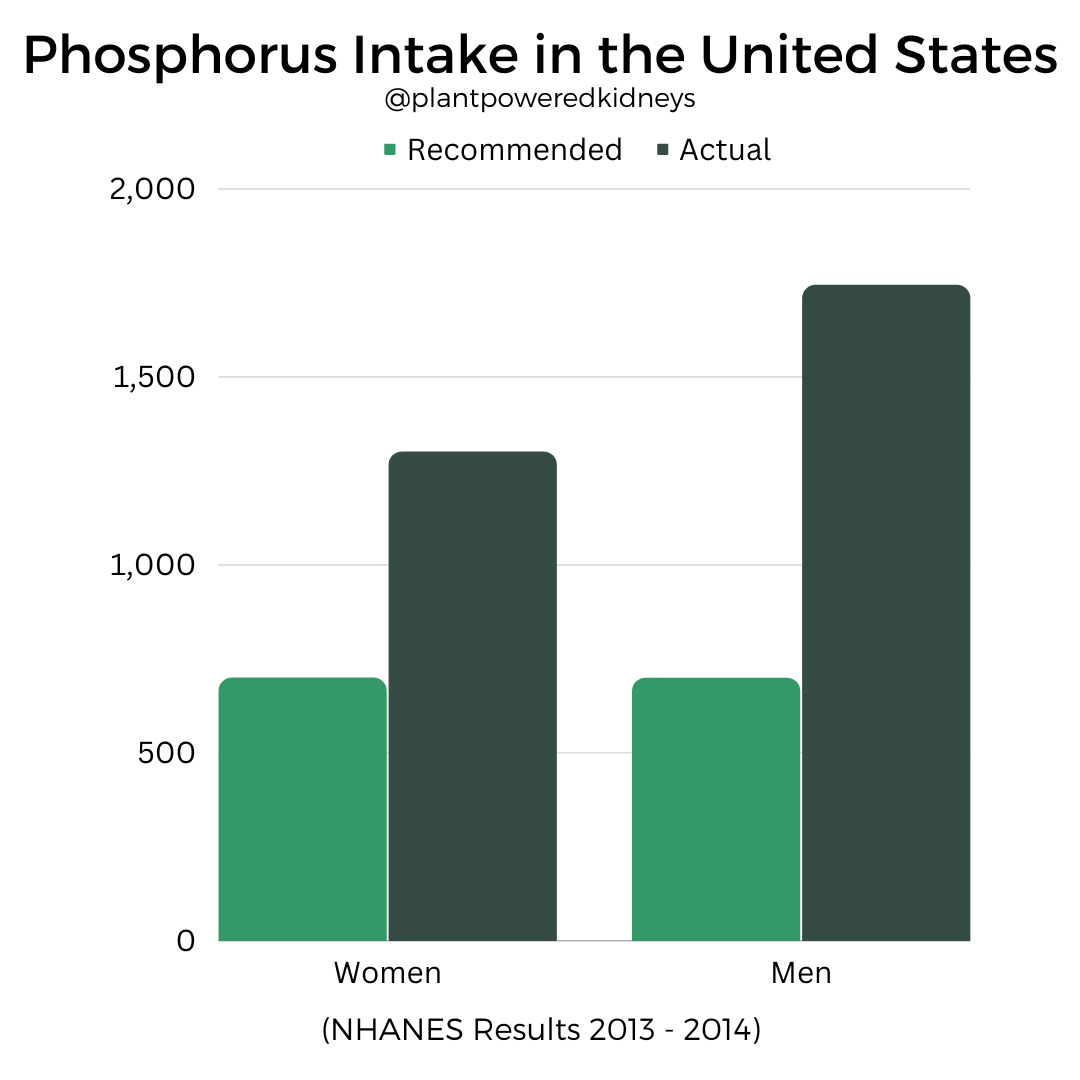
According the National Health and Nutrition Examination Survey (NHANES) in 2013-2014, men consumed on average 1,744 milligrams per day.
Women consumed 1,301 milligrams per day.
While this doesn’t specify kidney disease versus non-kidney disease, it is safe to say the general population eats plenty of phosphorus.
Recommended Daily Intake of Phosphorus for Kidney Disease
It’s recommended those with kidney disease keep phosphorus intake between 700-1,200 milligrams per day.
Some may have stricter guidelines based on personal lab results.
However, what’s most important is where the phosphorus comes from.
Phosphorus Levels in the Blood
Normal phosphorus levels should be around 2.5 – 4.5 mg/dL.
You may find this in your renal function panel.
However, you may need to ask for your phosphorus level to be checked by your doctor or nephrologist.
The goal range of phosphorus for dialysis patients is 3.0 – 5.0 mg/dL.
This slightly higher range is provided due to the challenge that comes with controlling phosphorus.
In end stage kidney failure, there is little- to no phosphorus excretion from the kidneys.
Additionally, limited phosphorus is removed from dialysis treatment.
Both too-low and too-high phosphorus levels increase the risk of death.
Those with uncontrolled phosphorus levels are often prescribed phosphorus binders.
How Does Kidney Disease Affect Phosphorus?
Phosphorus is one of the considerations in discussing a renal diet and kidney disease.
This is because as kidney function declines, so does its ability to safely manage phosphorus levels.
In later stages of CKD, phosphorus can tend to rise. This is for several reasons.
One is that the parathyroid hormone (PTH) can increase with kidney disease.
It pulls both calcium and phosphorus from the bones and into the bloodstream.
Another reason is that many people with kidney disease eat foods that are, unknowingly, high in phosphorus.
For this reason, a low phosphorus diet may be advised.
Too Much Phosphorus in the Diet Leads to High Phosphorus Levels
When phosphorus levels in the blood are above normal range, it is known as hyperphosphatemia.
Damage from CKD and other kidney disorders like polycystic kidney disease weaken kidneys leaving them unable to properly filter phosphorus.
Eating a large amount of foods high in inorganic phosphorus will also elevate blood levels of this nutrient.
As a result, further damage to the kidneys and overall health will ensue.
Too Much Phosphorus Can Be Dangerous
It is important to be in a safe zone when it comes to phosphorus.
According to the National Kidney Foundation, too much of this nutrient is dangerous to the body.
As a patient with CKD, it is important to learn how to manage your phosphorus levels.
If you don’t know your status, ask a member of your healthcare team where your phosphorus level is on your blood test results.
Write the number down and keep track of how it’s doing from that point.
Better yet- grab our free lab tracker below.
Signs of High Phosphorus
One way to tell if you have high blood phosphorus is to be on the lookout for symptoms of high phosphorus.
They include:
- High blood pressure
- Weakened bones
- Low vitamin D status
- Reduced calcium levels
- Muscle pain, cramps or spasms
- Numbness or tingling around the mouth
- Bone and joint pain
- Rash
- Itching
- Weakness
- Rash/bumps on the skin
- Red, itchy eyes
- Constipation
- Nausea
- Vomiting
- Diarrhea
Elevated phosphorus levels can also result in calcium deposits.
These calcium deposits will form in the blood vessels, lungs, eyes, and heart.
This can increase your risk of cardiovascular disease, stroke, and death.
These side effects of high phosphorus are not visible. Consequently, they are only discovered through clinical lab testing.
A medical condition known as calciphylaxis can also be caused by high phosphorus levels.
This condition is very dangerous, painful, and deadly if left untreated.
What Happens If Phosphorus Gets Too Low?
Symptoms of low phosphorus (aka hypophosphatemia) can include:
- Loss of appetite
- Bone pain
- Fragile bones/Fractures
- Joint pain
- Fatigue
- Numbness
- Confusion
- Muscle weakness
But don’t worry about not getting enough. It is rare to have a phosphorus deficiency.
As we mentioned earlier, phosphorus is incredibly common in our diet.
It’s a much bigger and more frequent concern to have too much phosphorus rather than not enough.
How to Lower Phosphorus Levels with Low Phosphorus Foods
Are you suffering from any of the symptoms above? Have you been told your phosphorus level is elevated?
Unfortunately, low phosphorus levels will not magically change all by themselves.
Like other aspects of kidney disease, lowering phosphorus levels requires a little work on your part.
The biggest factor influencing phosphorus is diet.
So if you’re left wondering what should I eat if my phosphorus is high?
Have no fear, the answer is simple.
Incorporate more low-phosphorus foods and know what to limit when it comes to high-phosphorus foods.
What Foods Contain Phosphorus?
To figure out how to lower your blood phosphorus we must first establish what are the foods that contain phosphorus.
Dietary phosphorus sources include both foods that naturally contain this mineral and those that have had it added during food processing.
The foods containing phosphorus include many food groups.
Some examples of organic phosphorus-rich foods are:
- Dairy
- Animal proteins
- Nuts
- Seeds
- Beans
- Grains

The body absorbs phosphorus in some foods more easily than others.
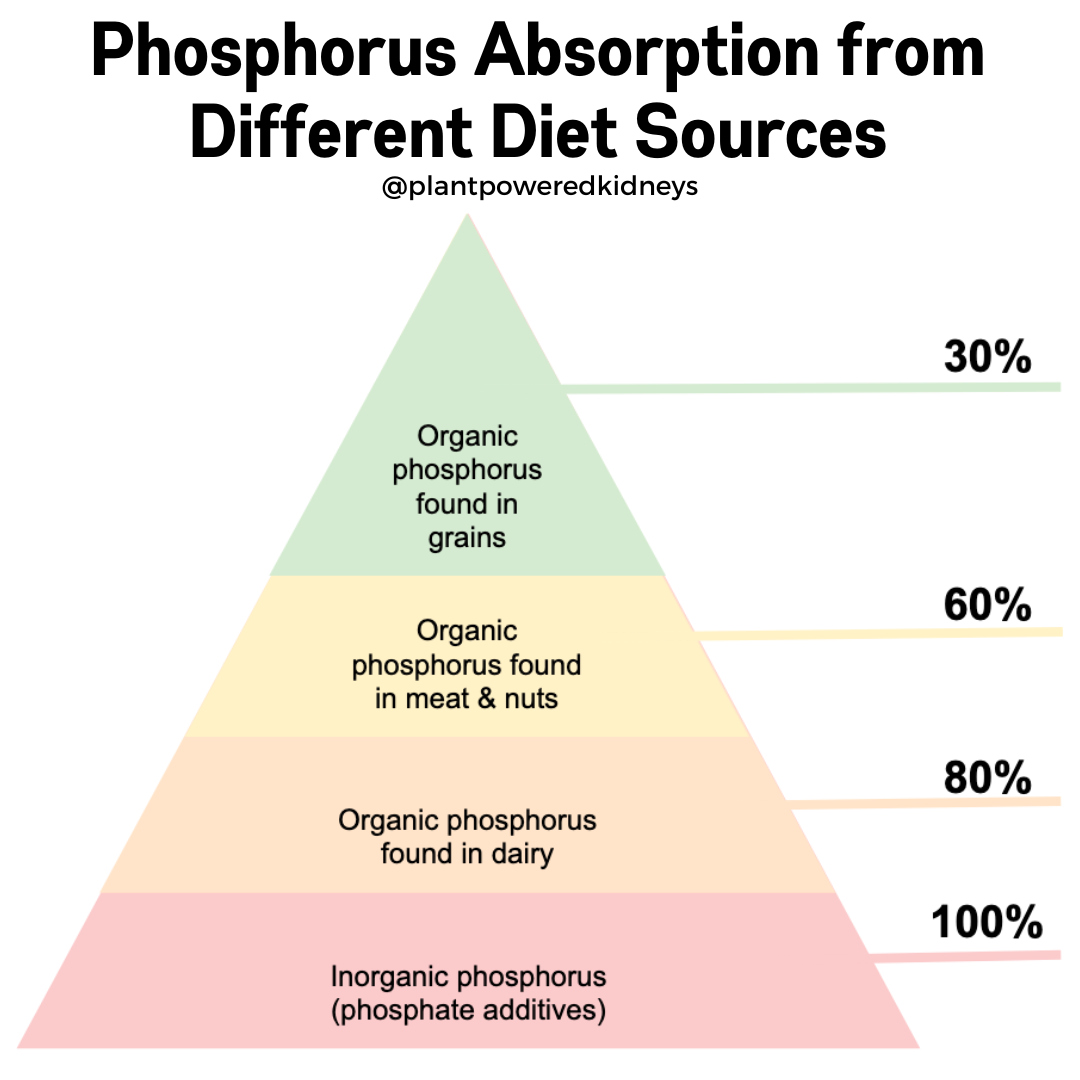
Grains that contain organic phosphorus is only absorbed by about 30 percent.
Therefore, even grains that are considered “high” in phosphorus aren’t truly as high as we thought they once were.


Animal sources of phosphorus have an absorption rate between 40 and 70 percent.
This is higher than plant sources.
Inorganic phosphorus is absorbed 90 to 100 percent.
This is the type of phosphorus that is most dangerous for kidney patients because it is so highly absorbed.
The phosphorus content of foods varies from high to low.
Below we will go over a list of both high and low phosphorus foods.
What Foods Are High in Phosphorus?
You may be wondering what foods to avoid if phosphorus is high?
This section will tell you exactly what you should steer clear of if you have high blood phosphorus.
We have put together a handy list of food high in phosphorus for your convenience.
High phosphorus foods include the following:
Foods High In Phosphorus Chart
| Food Group | Organic Phosphorus Absorption | Food List |
|---|---|---|
Dairy | 80% | Ice cream Hard Cheeses Custard Milk Cottage cheese Yogurt (not Greek) Pudding Cream soups |
| Beverages | *90 – 100% | Cocoa Ale/ Beer Chocolate drinks Dark colas with milk Canned/ bottled iced teas Pepper-type soda (Dr. Pepper) |
| Animal Protein foods | 60% | Oysters Sardines Beef liver Chicken liver Fish roe Organ meats |
| Other | 90 – 100% | Processed foods Prepared foods Deli meats Hot dogs Bacon Sausage Pizza Brewer’s yeast |
Phosphorus Additives
Some of the other foods highest in phosphorus include those with phosphate additives.
They will contribute between 300 and 1,000 mg of phosphorus to the diet.
Approximately between 70 and 100 percent of inorganic phosphorus is absorbed when these substances are consumed.
Drinks and foods with phosphate additives are those that have phosphorus added during processing.
How to Find High Phosphorus Foods
To check the food for inorganic phosphorus all you have to do is look at the ingredient list.
If you see the words “PHOS” it means the food contains a phosphorus additive.
Here is a list of common phosphate additives added to foods:
- Dicalcium phosphate
- Disodium phosphate
- Monosodium phosphate
- Phosphoric acid
- Sodium hexameta-phosphate
- Trisodium phosphate
- Sodium tripolyphosphate
- Tetrasodium pyrophosphate
You want to limit or avoid high phosphorus foods, especially phosphate additives, as much as possible.
Instead, focus on adding more low-phosphorus foods to the diet.
This can include grains, nuts and seeds due to the low absorption of phosphorus.
What Foods Are Low in Phosphorus?
To keep phosphorus levels in check and prevent any further kidney damage, you need to start a low phosphorus diet.
This means adding more low phosphorus foods into your meals.
To make this more digestible (pun intended) for you below we will discuss the various categories of foods with low phosphorus.
They are:
- Vegetables
- Fruit
- Dairy
- Meats and Poultry
- Fish
- Grains, Breads, and Pasta
- Beans & Legumes
- Nuts & Seeds
- Beverages
- Snack foods
- Foods low in phosphate additives
Low Phosphorus Vegetables
If you’re wondering which vegetables are low in phosphorus, the answer is basically all of them.
As mentioned, the organic phosphorus content of vegetables is poorly absorbed.
This means the phosphorus in vegetables will not likely impact your phosphorus levels.
It’s important to look at ingredient lists when you are choosing canned or otherwise packaged and processed vegetables.
Low phosphorus vegetables can become high phosphorus vegetables if they contain phosphate additives.
For a complete list of vegetables low in phosphorus check out this renal grocery list.
Low Phosphorus Fruits
Foods low in phosphorus include fruits.
The concept is the same for fruits as it is for vegetables.
This means fresh fruits are naturally low phosphorus foods.
Canned, packaged, and preserved fruits may be high in phosphorus if they have added phosphates in the ingredients list.
As a result, packaged/processed fruits should be avoided if phosphorus control is an issue.
Low Phosphorus Beans & Legumes
The old renal diet told us that beans and legumes were high in phosphorus.
What we know now is that beans and legumes have organic phosphorus that we cannot digest or absorb well.
The absorption rate of beans and legumes is approximately 30 – 60% of what you will see on nutrition facts.
Beans and legumes like the following may be included in a low phosphorus diet:
- Baked beans
- Black beans
- Butter beans
- Chickpeas / Garbanzo beans
- Edamame
- Kidney beans
- Lentils
- Lima beans
- Northern beans
- Pork and beans
- Split peas
- Soybeans
Keep in mind we are addressing the organic phosphorus that is naturally found in beans and legumes.
It’s important to read the ingredient list to identify any inorganic phosphorus when choosing canned or processed beans or legumes.
For more information about beans and potassium, here’s another article.
Low Phosphorus Dairy
As mentioned above, the absorption of dairy is approximately 80% of what you will find on a nutrition label.
Though a lot of dairy is not compliant with a low phosphorus diet, there are certain low phosphorus cheeses, yogurts, and other dairy products that are ok to eat.
Here are some dairy products that are lower in phosphorus:
Phosphorus in milk is generally higher and easily absorbed.
Cow’s milk contains approximately 230 – 260 milligrams of phosphorus per 8 oz cup.
At an 80% absorption, this still puts milk on the higher end at 184 – 208 milligrams of phosphorus per cup.
Rice milk and almond milk are two low phosphorus foods that can substitute in place of cow’s milk.
Read more about milk and kidney disease in this post.
Low Phosphorus Meats and Poultry
Remember, organic phosphorus that is naturally in meats is absorbed by about 60%.
Low phosphorus meats and poultry include the following foods:
- Chicken
- Turkey
- Fish
- Beef
- Veal
- Egg whites
- Lamb
- Pork
However, many types of meat have injections and additives that can include phosphorus.
Be sure to read the label.
If ordering at the butcher counter, ask if there have been any flavor enhancements or preservatives added to the meats.
Warning: they won’t always know what has been put in the meats.
This is why meats may seem low in phosphorus when they are actually not.
Low Phosphorus Fish & Seafood
Fish and seafood are low phosphorus foods that can be added to your diet.
Fish that have been recommended include:
- Canned (phosphate additive free) tuna and salmon
- Fresh cod, haddock, salmon, tuna
- Fish sticks (no phosphate added)
- Crab sticks
Frozen fish and seafood often have added phosphates used as preservatives.
Again, this is not recommended and would not be considered a low phosphorus food.
Low Phosphorus Pasta, Grains, and Breads
Whole grains may be high in phosphorus, their low absorption rate makes them qualify as a low phosphorus food.
The phosphorus in whole grains is only absorbed by about 30%.
These foods also offer fiber which is an essential nutrient for kidney disease and its associated health conditions.
Feel free to add pasta, grains, and breads like these to your diet:
- Pasta
- Brown rice
- Wild rice
- Whole wheat bread bagels, and buns
- Oats
- Quinoa
- Farro
- Freekeh
- Amaranth
- Sorghum
- Tapioca
- Millet
- Barley
- Bulgur
- Kamut
- Durum
- Buckwheat
- Teff
- Arrowroot
- Wheat berries
- Couscous

Low Phosphorus Beverages
When we think of low phosphorus foods we may not take into account the phosphorus in our beverages.
Therefore, it is important to look at what you are drinking to avoid any added phosphorus from beverages.
To limit your phosphorus, incorporate these drinks instead:
- Water
- Coffee
- Tea
- Rice milk (unenriched)
- Apple juice
- Cranberry juice
- Grape juice
- Lemonade
- Ginger ale
- Lemon lime soda
- Orange soda
- Root beer
Read more about kidney-friendly drinks in this post.
Low Phosphorus Snacks
Just because you have kidney diseases does not mean you can’t indulge in a snack every once in a while.
The problem with many snack foods is they contain inorganic phosphorus.
Ultimately, they will have an unhealthy amount of phosphorus.
This snack list offers low phosphorus foods to keep your blood phosphorus regulated:
- Rice cakes
- Pretzels unsalted
- Popcorn unsalted
- Crackers unsalted
- Poundcake
- Sugar cookies
- Chocolate
Yes, even chocolate is considered low in phosphorus.
This is because the natural phosphorus found in chocolate is not highly absorbed.
For more snack ideas that include low phosphorus foods, check this article.

Low Phosphorus Meal Plan
If you’re looking for a kidney-friendly meal plan that focuses on low phosphorus foods, we have a free PDF download for you here.
Our free meal plan includes nutrition information for all recipes, plus full nutrition tallies (including phosphorus) for each day.
We will also send you emails to continue to teach and support you with adding more low phosphorus foods and kidney-friendly meals that protect your kidney health.
Phosphorus Levels Affects Other Nutrient Levels
The thing to remember about nutrients in the body is that they work in tandem sometimes. So the levels of one mineral can affect another.
Three nutrients that are affected by phosphorus include:
- Calcium
- Potassium
- Sodium
Calcium and Phosphorus
Earlier we briefly talked about how elevated phosphorus levels can lead to a reduction in calcium.
This is dangerous for bone health.
When phosphorus is high the body will want to correct its calcium level.
So then the body will take calcium from the bone to compensate for the low blood levels.
As phosphorus levels rise calcium will continue to be taken and bone health is at risk.
The recommended calcium to phosphorus ratio should be 2 to 1.
Preventing bone breakdown starts with getting low phosphorus foods and adequate calcium in the diet.
Potassium and Phosphorus
The relationship between potassium and phosphorus is less known than that of calcium and phosphorus.
However, some research showed a low potassium diet could also impact bone health.
So anyone with an intake of low phosphorus and potassium foods needs to make sure they get enough nutrients to compensate for potential bone problems.
Read more about a low potassium diet here.
Phosphorus and Sodium
The relationship between phosphorus and sodium is different from other nutrient interactions.
Instead, it is the effects when these two electrolytes are combined that are of importance.
The mixture of phosphorus and sodium is very harmful to people with CKD.
Excess intake of these nutrients can lead to heart and bone disease.
Read more about a low sodium diet here.
Additional Ways to Lower Phosphorus Levels
Sometimes incorporating low phosphorus foods may now be enough to reduce phosphorous levels.
Additional interventions may be needed. They include:
- Medications
- Dialysis
- A kidney transplant
Phosphorus Medication Helps Lower Phosphorus Levels
Phosphorus medication can be given to lower phosphorus levels.
They are called phosphate binders. These should be taken with meals and snacks.
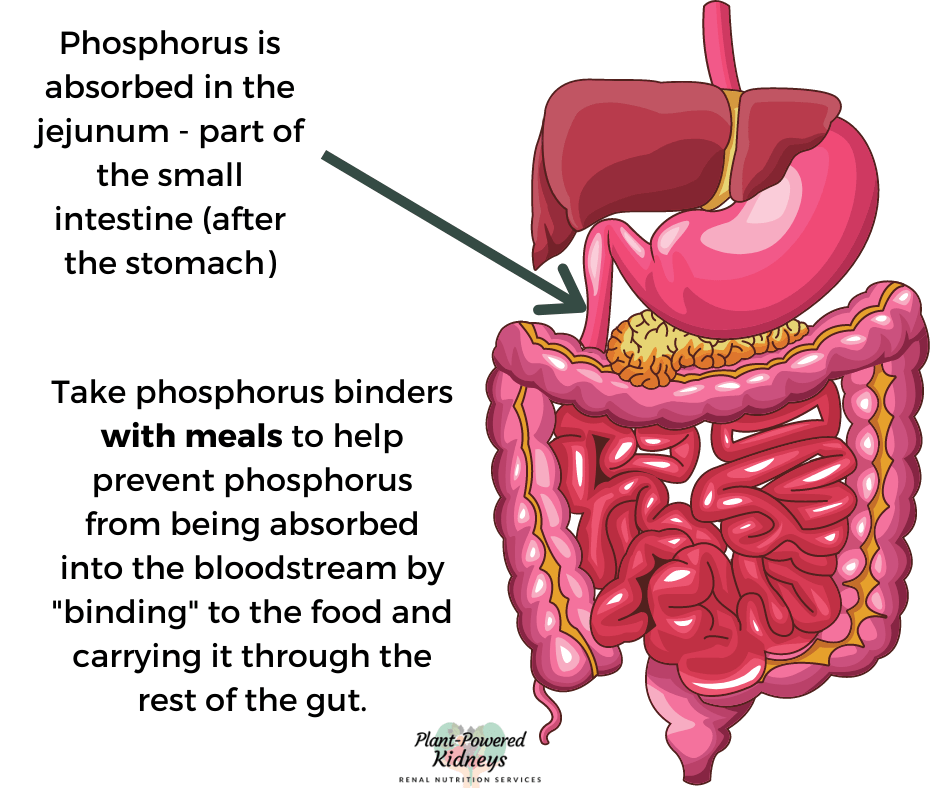
A phosphate binder will bind to the phosphorus in food eaten.
This will reduce how much phosphorus is absorbed by the body.
As a result, phosphorus levels will become regulated.
They come in a pill, chewable tablet, powder, or liquid form. Some examples of phosphate binders include
- calcium carbonate
- calcium acetate
- sevelamer hydrochloride
- lanthanum carbonate
- magnesium hydroxide
Natural phosphorus binders are made from food or vitamins.
Niacin, nicotinamide, and chitosan chewing gum fall into this category.
The research has not proved these products to be as effective as other phosphate binders.
Consequently, there are also side effects of phosphate binders.
They include nausea, diarrhea, constipation, abdominal pain, gas, and changes in stool color.
Side effects are often seen with initial use and will often subside after a few weeks.
Some binders also contain calcium, while others do not.
Phosphate binders should only be taken under the supervision of your doctor or renal RD.
If you are curious about these medications ask your healthcare team to know if binders are right for you.
Learn more about phosphate binders in this post.
Dialysis Can Help Lower Phosphorus Levels
Dialysis will also remove some phosphorus from the blood.
However, you still need to regulate phosphorus levels between dialysis treatments to prevent phosphorus buildup.
Therefore, you still may need to implement low phosphorus foods into the diet.
Ask your doctor and renal dietitian what you should be doing between dialysis treatments if you are on dialysis and still have high phosphorus levels.
A Kidney Transplant Can Lower Phosphorus Levels
Having a kidney transplant can also lower phosphorus levels.
In fact, many kidney transplant recipients are encouraged to eat more high phosphorus foods after a transplant.
This is because kidney transplant patients have functioning kidneys that will manage the phosphorus levels well.
A Renal Dietitian Can Help with Low Phosphorus Foods
If you’re wondering how much phosphorus is allowed on a renal diet. It depends on the person.
Your renal dietitian can help determine your phosphorus needs. If you have a restriction they will help you find low phosphorus foods and create a meal plan that is just right for you.
Learn about working with a dietitian at Plant-Powered Kidneys here.
Summary
Phosphorus is an essential nutrient that is found in foods and is also added during food processing. It is needed by the body to produce energy, maintain bone health, regulate DNA, and balance pH levels.
Phosphorus levels depend on the kidneys’ filtration system. Unfortunately, damage from health conditions like CKD causes high levels of phosphorus to build up in the blood.
Foods lowest in phosphorus are natural foods. Some may contain organic phosphorus, like beans, nuts, seeds, and grains. However, the body cannot digest it.
Foods highest in phosphorus have inorganic phosphorus, which is highly absored. This comes in the form of phosphate additives. Finding additives with phosphorus can be done by reading the ingredient list for the letters “phos” in an ingredient. A common example of this is phosphoric acid.
As a result, individuals with kidney damage need to limit their intake of foods high in phosphorus. One way to regulate phosphorus levels is through consuming more low phosphorus foods. These can be found among all food groups and can be easily integrated into the diet with the help of your renal dietitian.
If diet alone is not cutting it you can talk to your healthcare team about additional treatments that may lower phosphorus levels and prevent the kidneys from further harm.
Jen Hernandez is a registered dietitian, board-certified specialist in renal nutrition, and author of Plant-Powered Kidney Nutrition: Proven Methods and Easy Recipes to Support Your Kidney Health (available on Amazon). She has nearly a decade of experience with kidney disease patients in all stages - from stage 1 through kidney transplant. Jen writes on the blog of Plant-Powered Kidneys to help reach and teach more kidney patients about how they can enjoy more foods in a plant-based diet while protecting kidney health.




Would you consider most beans to be high in phosphorus? Or just the ones you’ve listed. I’m curious about pinto beans specifically.
Beans are considered moderate to high in phosphorus. However (and it’s an important however), the phosphorus that is naturally in beans is organic and therefore not well absorbed. Many people in all stages of CKD can enjoy beans in their diet. 🙂
What about potatoes? I haven’t seen them mentioned in any article I’ve read. BTW, I’m a newly diagnosed CKD patient trying to learn to live. Thanks for the information!
Potatoes are mostly associated with potassium- and are quite high in potassium. Check out this article about the low potassium diet!
Hi Jen, I eat potatoes, we soak them in water or double boil them. Also my phosphorus levels have gone up and think it was caused by drinking various coffee creamers and I eat grain breads a couple of times a day. Delores Lubbes
Hi Delores! So good to hear from you. I love that you investigate the cause behind your phosphorus levels. That’s a great way to stay on top of it! As you can see from this article, grains aren’t generally a cause of high phosphorus.. unless they’ve added phosphates to a pre-packaged/pre-seasoned item. Wishing you the best💚
Hello Jen,
Thank you for all your insightful information. I’m wondering how dried beans soaked and cooked in a crock pot are valued for phos, potassium and sodium intake? Is there a few choices of dried beans that work out overall better than other choices? Also, are bean pastas, for example, chickpea bean pasta a better choice over regular white pastas?
Hi Barbara, thanks for your kind words! I cited a research paper in this other article about beans that found potassium was slightly reduced after soaking and pressure-cooking. This research noted that potassium and phosphorus CKD guidelines needed to be updated, which they later were.
I also have an article about pastas and briefly discuss bean/legume pastas there as well. The term “better” is subjective, depending on a persons nutritional goals and allowances.
I hope this helps!